Postural kyphosis represents one of the most common sagittal plane spinal deformities, particularly among adolescents and increasingly in sedentary adults. Unlike structural kyphosis—such as Scheuermann’s disease, which involves anterior wedging of the vertebrae—postural kyphosis is characterized by a flexible, non-congenital increase in the thoracic curve (1, 2). From an osteopathic and rehabilitative perspective, this condition is viewed not just as a spinal curve, but as a global disruption of the "odontoid-hip axis" (OD-HA) and the body's center of mass (3, 4).
Pathophysiology and the "Paramorphism" Concept
In earlier literature, postural deviations like kyphosis were often referred to as paramorphisms—alterations in form that do not yet involve permanent structural damage to the bone or ligaments (5). In the context of postural kyphosis, the deformity is often secondary to:
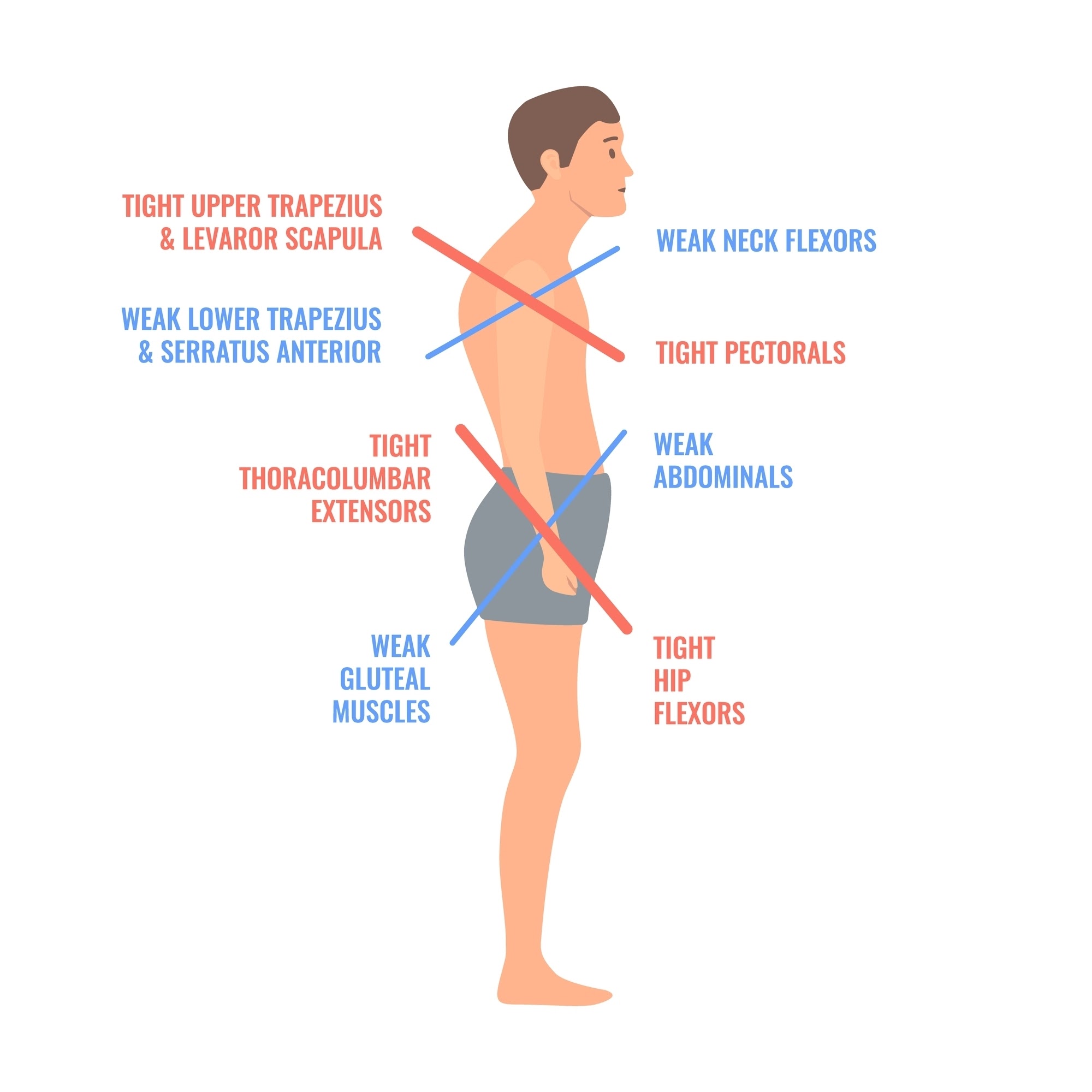
Muscular Imbalance: Weakness in the spinal extensors (erector spinae) and mid-back stabilizers (rhomboids, trapezius) contrasted with tightness in the anterior chain (pectoralis major and minor).
Evolutionary Instability: The upright posture requires constant neuromuscular calibration to maintain horizontal gaze; when this fails, the trunk naturally collapses into a kyphotic state (1).
Compensatory Patterns: Increased thoracic kyphosis rarely exists in isolation. It frequently triggers a "rounded shoulder" appearance and forward head posture, a triad often analyzed in studies of Upper Crossed Syndrome (6).
Osteopathic and Manual Therapy Principles
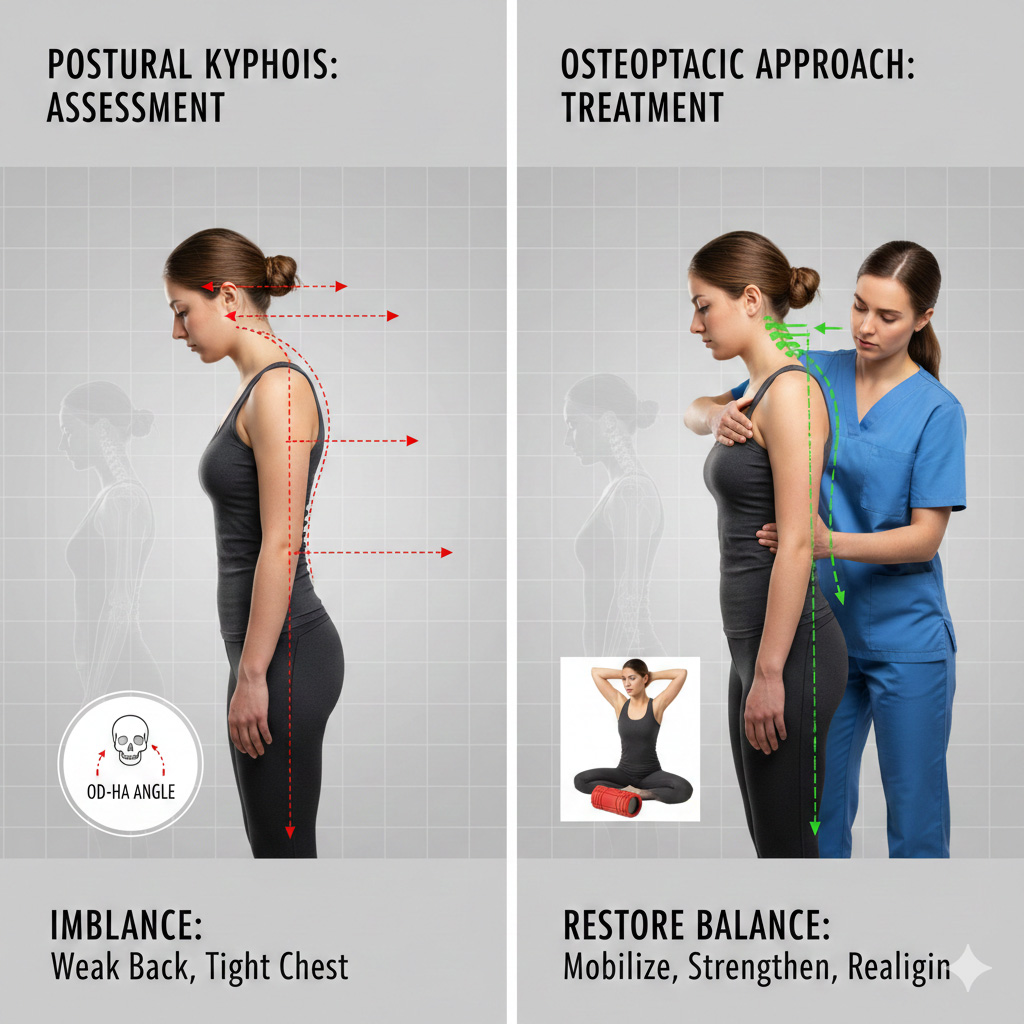
Osteopathic management of postural kyphosis focuses on restoring the functional "sagittal balance." This involves more than simply "straightening" the back; it requires addressing the entire kinetic chain.
Effective treatment begins with an understanding of global alignment. Modern analysis suggests that the odontoid-hip axis (OD-HA) is the most efficient parameter for determining how well a patient is balanced (4). Osteopathic practitioners look for "barycentric" shifts—how the patient's center of mass has moved in relation to their base of support (3). If the thoracic kyphosis shifts the center of gravity forward, the patient may compensate through pelvic tilts or knee flexion, which must also be addressed.
The goal of manual intervention is to convert a "stiff" kyphosis back into a flexible "postural" one.
Anterior Chain Liberation: Addressing the "Pillow Case" phenomenon—where severe kyphosis limits thoracic expansion—requires stretching the intercostal muscles and pectorals to allow for better lung capacity and upright positioning (7).
Segmental Mobility: Osteopathic manipulative treatment (OMT) aims to improve the mobility of the thoracic vertebrae and the rib cage, reducing the "hump" appearance and alleviating the compensatory strain on the cervical and lumbar spine (2).
Evidence-Based Exercise Interventions
The literature consistently highlights that manual therapy must be paired with targeted strengthening to achieve lasting results.
The Study of Hyperkyphosis, Exercise, and Function (SHEAF) demonstrated that a dedicated spine-strengthening program significantly reduces kyphosis angles (8). This confirms the osteopathic theory that restoring the "tension" in the posterior myofascial lines is essential for maintaining the correction achieved through manual manipulation.
Recent systematic reviews have confirmed that therapeutic exercises are highly effective for Upper Crossed Syndrome. These interventions typically result in significant improvements in:
Thoracic kyphosis angles.
Forward head posture (Craniovertebral angle).
Rounded shoulder posture (6, 9).
Clinical Implications: Beyond the Spine
Failure to treat postural kyphosis can lead to systemic issues. In geriatric populations, severe kyphosis can interfere with medical care, such as the ability to lie flat for surgery (7). In neurological contexts, such as Parkinson's Disease, increased kyphosis (camptocormia) is a direct contributor to shoulder stiffness and adhesive capsulitis, as the altered scapular position impinges on the glenohumeral joint (10).
Conclusion
Postural kyphosis is a reversible functional disturbance that responds well to a combination of osteopathic manual therapy and corrective exercise. By focusing on the OD-HA angle and the restoration of sagittal balance, clinicians can move beyond treating a "slouch" to treating a global postural dysfunction. The synergy of mobilizing restricted joints and strengthening the posterior chain remains the gold standard for non-surgical kyphosis management (11).
References
Abelin-Genevois K. Sagittal balance of the spine. Orthop Traumatol Surg Res. 2021 Feb;107(1S):102769.
Negri V, Marenghi P. [Juvenile kyphosis]. Acta Biomed Ateneo Parmense. 1984;55(2):113-8. Italian.
Khalifé M, Vergari C, Assi A, Guigui P, Attali V, Valentin R, et al. Full-body Postural Alignment Analysis Through Barycentremetry. Spine (Phila Pa 1976). 2024 Dec 1;49(23):1652-1660.
Le Huec JC, Thompson W, Mohsinaly Y, Barrey C, Faundez A. Sagittal balance of the spine. Eur Spine J. 2019 Sep;28(9):1889-1905.
Stolfi P. [Paramorphisms]. Minerva Med. 1975 Sep 22;66(62):3156-7. Italian.
Sepehri S, Sheikhhoseini R, Piri H, Sayyadi P. The effect of various therapeutic exercises on forward head posture, rounded shoulder, and hyperkyphosis among people with upper crossed syndrome: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2024 Feb 1;25(1):105.
Gordon MI, Rodríguez AA, Olson MD, Miller KM. Pillow case. J Cataract Refract Surg. 2005 Sep;31(9):1824-5.
Katzman WB, Vittinghoff E, Lin F, Schafer A, Long RK, Wong S, et al. Targeted spine strengthening exercise and posture training program to reduce hyperkyphosis in older adults: results from the study of hyperkyphosis, exercise, and function (SHEAF) randomized controlled trial. Osteoporos Int. 2017 Oct;28(10):2831-2841.
Porto AB, Nascimento Guimarães A, Alves Okazaki VH. The effect of exercise on postural alignment: A systematic review. J Bodyw Mov Ther. 2024 Oct;40:99-108.
Papalia R, Torre G, Papalia G, Baums MH, Narbona P, Di Lazzaro V, et al. Frozen shoulder or shoulder stiffness from Parkinson disease? Musculoskelet Surg. 2019 Aug;103(2):115-119.
Pizzutillo PD. Nonsurgical treatment of kyphosis. Instr Course Lect. 2004;53:485-91.