Introduction
Scheuermann’s disease—also known as Scheuermann’s kyphosis—is the most common structural cause of hyperkyphosis in adolescents. First described by Holger Scheuermann in 1920, the condition is characterized by vertebral wedging, endplate irregularities, and progressive thoracic or thoracolumbar kyphotic deformity. Although classically considered a benign and self-limited disorder, more recent studies highlight the range of biomechanical, psychosocial, and long-term functional implications associated with the disease. Postural kyphosis also commonly occurs during periods of rapid growth and development. Compared with this disease, the deformity is more reversible and the prognosis is better. Early and accurate diagnosis is beneficial for targeted treatment.
Recent literature—including updated radiological classifications, biomechanical models, and evolving surgical indications—has expanded understanding of the etiology, diagnosis, and management of Scheuermann’s disease. This review synthesizes key findings from eight major sources, including contemporary radiological updates (Kaur & Lalam, 2023), European orthopedic perspectives (Diaremes et al., 2022), and foundational clinical works (Lowe, 1990 & 1999), as well as more modern surgical guidelines (Sardar et al., 2019).
Epidemiology and Clinical Presentation
Scheuermann’s disease most commonly affects adolescents during periods of rapid growth. Reported prevalence ranges from 0.4% to 10%, with variations attributable to diagnostic criteria and population characteristics. Males are affected slightly more often than females, although some reports show equal distribution.
The condition frequently presents between ages 10 and 17. Patients commonly report:
-
Progressive postural kyphosis unresponsive to voluntary correction
-
Thoracic back pain aggravated by activity
-
Stiffness and fatigability of the back muscles
-
In severe cases, cosmetic concerns affecting self-image
-
Occasionally, compensatory lumbar hyperlordosis
-
Rarely, neurologic symptoms due to spinal cord compression (Lowe, 1999; Ali et al., 1999)
Pain is often the earliest symptom and tends to worsen with prolonged sitting, standing, or physical exertion. However, many young patients are asymptomatic and identified via screening or evaluation for postural abnormalities.
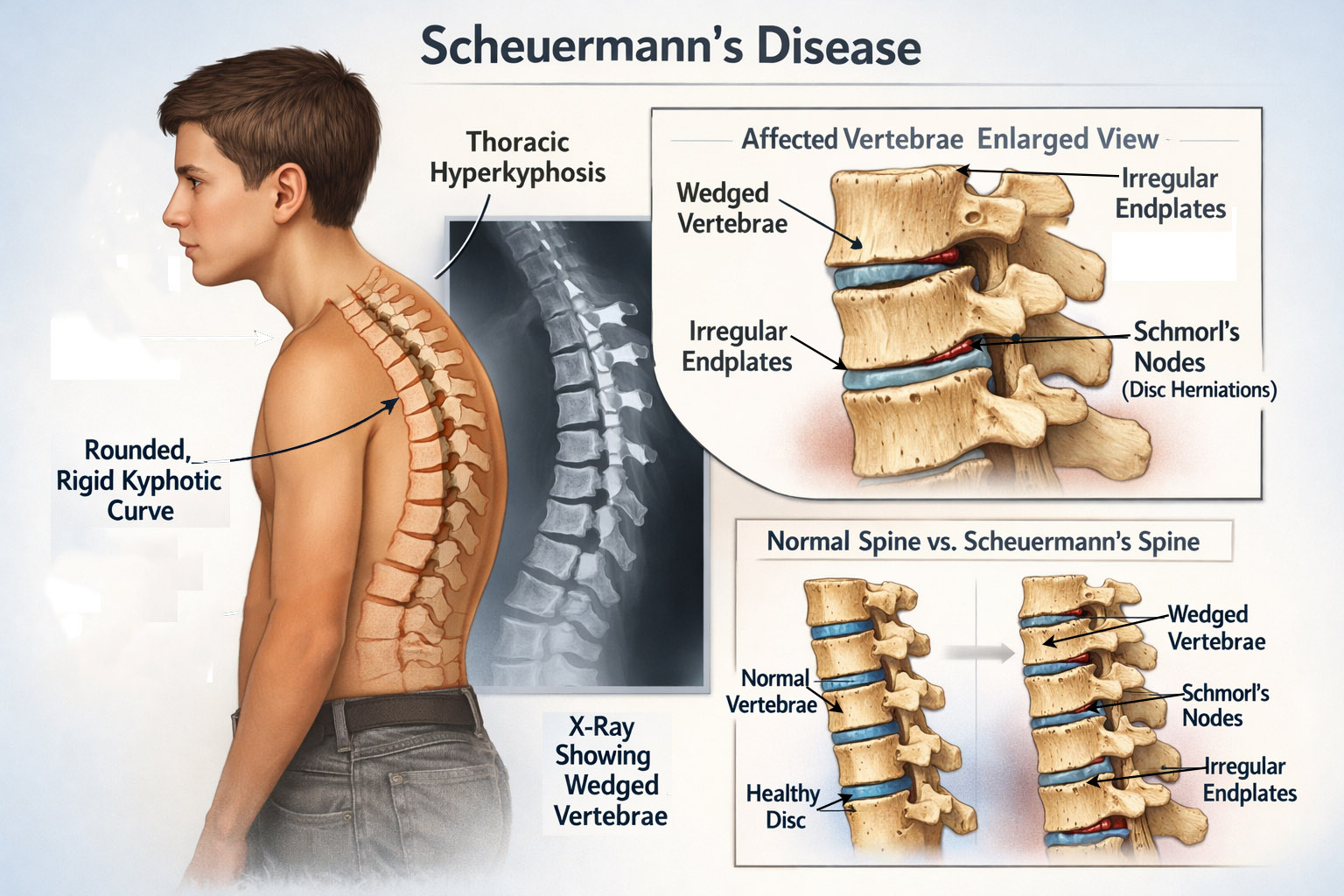
Pathophysiology and Etiology
The precise pathogenesis of Scheuermann’s disease remains unclear; however, several mechanisms have been proposed.
A dominant hypothesis is the presence of a disorder affecting the cartilaginous endplates of vertebral bodies. Microfractures, insufficient vascularity, or structural weakness of the endplate may lead to anterior vertebral body growth retardation, producing wedging. Histological studies demonstrate irregular endplate architecture, increased collagen content, and decreased mineralization (Lowe, 1999; Palazzo et al., 2014).
Repeated flexion loading during growth may contribute to overload of the anterior vertebral region. Athletes involved in high-impact or repetitive flexion sports—e.g., gymnastics, rowing, wrestling—show higher prevalence of vertebral endplate irregularities (Diaremes et al., 2022).
Although a precise genetic pattern has not been identified, familial clustering is well documented. Twin studies and pedigree analyses suggest a hereditary predisposition, likely polygenic.
Intervertebral disc herniations, Schmorl’s nodes, and degeneration appear frequently in affected segments, supporting the theory of mechanical overload combined with endplate weakness.
Weakness of spinal extensors and tightness of pectoral muscles may exacerbate postural changes, though these are considered secondary to structural deformity rather than primary causes.
Radiologic Features and Diagnosis
Scheuermann’s disease diagnosis traditionally requires:
-
Anterior wedging of ≥5° in at least three consecutive vertebrae
-
Endplate irregularities
-
Schmorl’s nodes
-
Thoracic kyphosis >45° (or thoracolumbar kyphosis exceeding normative values)
These radiographic features were refined over decades, with current criteria based on the original descriptions of Sorensen.
Kaur & Lalam (2023) provide an updated radiological interpretation, highlighting:
-
Improved MRI characterization of disc-endplate interactions
-
Differentiation between Scheuermann’s disease and postural kyphosis
-
Use of axial imaging to assess canal compromise in severe cases
-
Early detection of vertebral body changes before significant wedging develops
MRI is particularly useful when evaluating pain or neurologic symptoms and identifying concomitant disc pathology.
Clinical Classification
-
Most common
-
Kyphotic apex between T7–T9
-
Cosmetically prominent deformity
-
Less associated with pain in adulthood
-
Apex between T10–T12
-
Often more painful
-
Greater risk of progression into adulthood
-
More biomechanical stress on the lumbar spine
Distinguishing rigid from flexible kyphosis is essential. Scheuermann’s kyphosis typically remains structurally rigid, unlike postural kyphosis, which self-corrects with extension or prone positioning.
Natural History
The natural course of Scheuermann’s disease varies depending on curve magnitude, location, and skeletal maturity.
Deformity often progresses during growth spurts due to mechanical vulnerability of the immature spine.
Although many patients improve symptomatically after skeletal maturity, some continue to experience:
-
Chronic back pain
-
Reduced spinal mobility
-
Cosmetic dissatisfaction
-
Fatigue from compensatory lumbar hyperlordosis
-
Early-onset disc degeneration at the thoracolumbar junction (Lowe, 1990; Palazzo et al., 2014)
Thoracolumbar curves are especially prone to pain persistence.
Differential Diagnosis
Conditions that mimic Scheuermann’s disease include:
-
Postural kyphosis
-
Vertebral fractures (e.g., compression fractures)
-
Congenital kyphosis
-
Inflammatory conditions (e.g., ankylosing spondylitis)
-
Metabolic bone disorders
-
Neuromuscular kyphosis
MRI can help distinguish inflammatory or malignant conditions when clinically indicated.
Nonoperative Management
Nonoperative management remains the cornerstone of treatment, particularly for skeletally immature patients or those with curves less than 70–75°.
Physical therapy focuses on:
-
Strengthening spinal extensors
-
Stretching anterior-chain musculature (pectoralis, hip flexors)
-
Postural training and ergonomic education
-
Core stabilization
Although PT alone rarely corrects fixed kyphotic angles, it may reduce pain and improve functional capacity.
Bracing is most effective in adolescents with flexible curves and remaining growth potential.
Indications:
-
Kyphosis 55°–80°
-
Risser 0–2 (substantial growth remaining)
-
Progressive deformity
Common brace types include the Milwaukee brace and modern thoracolumbar orthoses. Evidence supports significant kyphosis reduction—averaging 10–15°—when compliance thresholds (≥16 hours/day) are met (Ali et al., 1999).
Pain, when present, is typically mechanical. Management may include:
-
NSAIDs
-
Activity modification
-
Avoiding prolonged flexion activities
-
Structured exercise programs
Activity is usually unrestricted unless pain dictates otherwise. High-impact sports may require temporary modification.
Surgical Management
Surgery is reserved for select cases and has evolved significantly over the past two decades. According to Sardar et al. (2019), the goals of surgery include:
-
Correction of kyphotic deformity
-
Pain reduction
-
Prevention of neurological compromise
-
Improvement of cosmetic appearance
-
Restoration of sagittal balance
Traditional criteria include:
-
Kyphosis >70–80° with documented progression
-
Persistent, severe pain unresponsive to conservative management
-
Neurologic deficit (rare)
-
Significant cosmetic or psychosocial impairment
-
Deformity causing cardiopulmonary compromise (very rare)
Modern instrumentation allows predictable correction with reduced morbidity, making POF the preferred approach today.
Advantages include:
-
Lower operative blood loss
-
Reduced complication rates
-
Shorter operative time
-
Comparable deformity correction to combined approaches
Previously the gold standard, this approach is now reserved for:
-
Very rigid curves
-
Severe deformity with sagittal imbalance
-
Rare cases where anterior release is required
Selecting optimal fusion levels is essential to minimize complications such as junctional kyphosis.
Sardar et al. (2019) recommend:
-
Incorporating the sagittal stable vertebra
-
Avoiding "short fusions" that increase biomechanical stress
-
Choosing end vertebrae based on neutral alignment and rotation
Modern series report:
-
Significant reduction in kyphotic angles
-
Durable correction with long-term follow-up
-
Reduced back pain
-
High levels of patient satisfaction
Complications, though reduced, may include:
-
Junctional kyphosis
-
Instrumentation failure
-
Neurologic injury (rare with modern monitoring)
-
Infection
Psychosocial Considerations
In addition to physical symptoms, Scheuermann’s disease may influence psychological well-being, especially among adolescents. Cosmetic concerns and peer perception may affect mental health, self-esteem, and social functioning. Early identification and empathetic communication play a key role in minimizing psychological burden.
Contemporary Updates and Research Directions
Recent advances have highlighted nuanced aspects of diagnosis and management:
Kaur & Lalam (2023) emphasize:
-
Enhanced MRI detection of early structural changes
-
Refined criteria for differentiating Scheuermann’s disease from inflammatory kyphoses
-
Improved risk stratification for treatment planning
Diaremes et al. (2022) provide updated German orthopedic guidelines that emphasize:
-
Earlier bracing when signs of vertebral wedging are emerging
-
Greater use of MRI for identifying endplate pathology
-
Distinguishing true Scheuermann’s disease from postural kyphosis with borderline radiographic findings
Recent work supports:
-
Evaluating sagittal alignment holistically, including pelvic parameters
-
Model-based prediction of curve progression
-
Identifying thoracolumbar variants at higher risk for pain
With improved surgical safety profiles, indications have broadened slightly—but remain reserved for severe or refractory cases.
Case Prognosis
-
Thoracic (vs. thoracolumbar) location
-
Kyphosis <70°
-
Good response to bracing
-
Minimal back pain
-
High compliance with physical therapy
-
Thoracolumbar involvement
-
Large curves (>75°)
-
Poor brace compliance
-
Marked endplate irregularities
-
Severe progressive deformity in adolescence
In adults, persistent pain is more likely with thoracolumbar disease and early degenerative changes.
Conclusion
Scheuermann’s disease is a complex structural spinal disorder characterized by rigid hyperkyphosis, vertebral wedging, and endplate abnormalities. While traditionally considered benign, the condition can cause significant pain, functional limitations, and psychosocial concerns. Diagnosis relies on characteristic radiographic findings, with MRI playing a growing role in early and differential diagnosis.
Management strategies range from observation and physical therapy to bracing and surgical intervention in severe cases. Modern posterior-only spinal fusion has become the surgical standard, offering reliable correction and improved safety.
Contemporary research continues to expand understanding of biomechanical, genetic, and radiological aspects of the disease, guiding more individualized and effective treatment strategies. With early recognition and appropriate management, the majority of patients achieve meaningful improvement and maintain good long-term functional outcomes.
References
-
Kaur S, Lalam R. Scheuermann's Disease. Semin Musculoskelet Radiol. 2023 Oct;27(5):522–528.
-
Diaremes P, Braun S, Meurer A. Scheuermann’s disease. Orthopade. 2022 Apr;51(4):339–348.
-
Lowe TG. Scheuermann's disease: an update. Orthop Clin North Am. 1999 Jul;30(3):475–487.
-
Palazzo C, Sailhan F, Revel M. Scheuermann disease. Joint Bone Spine. 2014 May;81(3):209–214.
-
Ali RM, Green DW, Patel TC. Scheuermann's kyphosis. Curr Opin Pediatr. 1999 Feb;11(1):70–75.
-
Sardar ZM, Ames RJ, Lenke L. Scheuermann's Kyphosis: Diagnosis, Management, and Selecting Fusion Levels. J Am Acad Orthop Surg. 2019 May;27(10):e462–e472.
-
Graham P. Scheuermann’s Kyphosis. Orthop Nurs. 2023 Jan–Feb;42(1):53–55.
-
Lowe TG. Scheuermann disease. J Bone Joint Surg Am. 1990 Jul;72(6):940–945.