Fryette’s Laws have been foundational in osteopathic education for describing predictable patterns of spinal coupling. They guide the interpretation of somatic dysfunction and help clinicians structure treatment. However, recent studies suggest the traditional model is more nuanced than once taught. Modern imaging, biomechanical analysis, and clinical research indicate that spinal movement varies widely between individuals and across regions of the spine. Understanding these updates allows practitioners to apply Fryette’s mechanics more accurately.
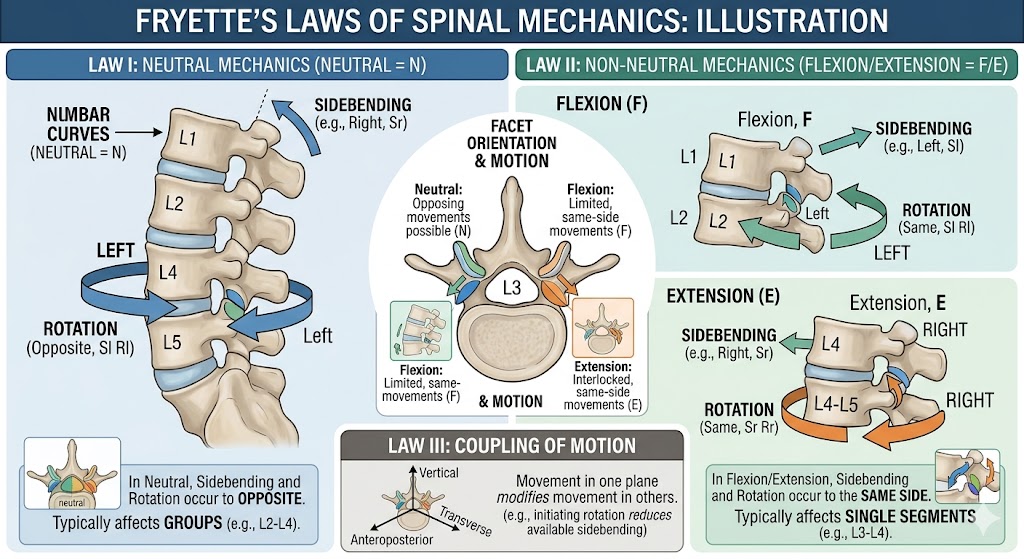
Classical Fryette’s Laws
Fryette described three key principles of spinal motion.
Law 1 proposes that in a neutral thoracic or lumbar spine, side-bending and rotation occur to opposite sides.
Law 2 states that in a flexed or extended spine, side-bending and rotation occur to the same side.
Law 3 suggests that introducing motion in one plane limits motion in the other two planes.
These laws remain useful conceptual tools for identifying patterns of dysfunction.
Modern Research and Evolving Understanding
Recent work by Haughton et al. (2024) (1) re-examined Fryette’s mechanics using static modeling. Their findings show that the actual angles of coupled spinal motion are often far smaller than expected. They concluded that the classical laws function best as simplified teaching models, not precise descriptions of real biomechanical behavior. Spinal movement is influenced by disc properties, facet orientation, ligament tension, and muscular patterns, which vary significantly between individuals.
A 2022 radiological study of cadaveric specimens by Siddiqi et al. (2) found that structural differences strongly influence how segments couple. The authors emphasized that physicians should integrate anatomical variability when applying Fryette’s Principles, especially when diagnosing dysfunction in the thoracic and lumbar spine. Their work reinforces the idea that Fryette’s patterns should guide—but not dictate—clinical reasoning.
Clinical relevance is highlighted in Lamberg et al.’s 2014 case report (3), which examined osteopathic assessment in a patient with severe scoliosis undergoing subarachnoid anesthesia. The study demonstrated that understanding Fryette mechanics remains vital when anatomical abnormalities are present. In such cases, appreciating how spinal curves and rotations deviate from classical patterns helps clinicians plan interventions safely, including procedural approaches such as neuraxial anesthesia.
Despite growing scientific nuance, Fryette’s model remains central in osteopathic practice. A national survey by Fryer, Morse, and Johnson (2009) (4) reported that 64% of osteopathic physicians document somatic dysfunction using Fryette nomenclature, and most rely on this framework during clinical decision-making. This reflects the continued value of Fryette mechanics as an essential language for describing spinal patterns, even as the profession refines its understanding.
Integrating Evidence into Clinical Practice
Modern research encourages clinicians to apply Fryette’s Laws with flexibility. They are best viewed as pattern-recognition tools rather than rigid biomechanical rules. Structural variations—such as degenerative change, scoliosis, or asymmetric facet orientation—may significantly alter coupling behavior. Careful palpation remains crucial, but when uncertainty arises, imaging can clarify anatomical influences on motion.
In practice, Fryette’s Laws support clinicians in forming a diagnostic framework, organizing findings, and communicating clearly in patient records. The modern evidence does not invalidate the laws; instead, it adds context that strengthens clinical interpretation and improves patient-centered decision-making.
Why This Matters for Patients
A refined understanding of spinal mechanics enables osteopathic practitioners to apply hands-on therapy more precisely. By integrating classical principles with modern research, clinicians can better interpret complex motion patterns, adjust treatment to individual anatomy, and enhance overall safety and effectiveness. At Dr. Ma's practice, we combine traditional osteopathic reasoning with the latest scientific insights to deliver accurate assessment and tailored manual therapy.
References
-
Haughton DR, Barr EC, Gupta AK, Toohey WC, Kania AM. Reassessing Fryette’s mechanics using static modeling. J Osteopath Med. 2024;124(10):429-435.
-
Siddiqi I, Wang A, Marino M, Bowen I, Miulli DE. Evaluation of Osteopathic Principles in Cadaveric Specimens Using Radiological Assessment. Cureus. 2022;14(12):e32120.
-
Lamberg JJ, Adhikary SD, McFadden AT. Osteopathic musculoskeletal examination and subarachnoid anesthetic administration in a patient with severe scoliosis. J Am Osteopath Assoc. 2014;114(7):582-585.
-
Fryer G, Morse CM, Johnson JC. Spinal and sacroiliac assessment and treatment techniques used by osteopathic physicians in the United States. Osteopath Med Prim Care. 2009;3:4.