Low back pain (LBP) is one of the most prevalent and disabling musculoskeletal conditions worldwide. The global burden is profound; according to major epidemiological analyses and the Lancet series, LBP is now recognized as the leading cause of years lived with disability, affecting individuals across all populations and socioeconomic groups.¹⁻² With lifetime prevalence rates approaching 84% and chronicity affecting nearly one quarter of adults at some point, LBP represents a condition of significant personal and societal importance.³ Understanding its mechanisms, clinical presentation, and management strategies is therefore essential.
Definition
Low back pain is defined as discomfort, tension, or stiffness localised between the lower rib margins and the gluteal folds, and may occur with or without radiating symptoms into the lower limbs.⁴ Clinicians frequently classify LBP as acute, subacute, or chronic depending on duration, and into specific or non-specific categories depending on whether a clear anatomical source of nociception can be identified. The literature repeatedly emphasizes that the vast majority of cases—up to 90%—are non-specific, with no identifiable structural lesion on clinical or imaging assessment.¹ LBP may also be conceptualized mechanistically as axial lumbosacral pain, radicular pain resulting from nerve root involvement, or referred somatic pain originating from spinal or paraspinal structures.² Mechanical low back pain, the most prevalent type, stems from the spine, intervertebral discs, and associated soft tissues but is often multifactorial.⁵
Definition
Low back pain is typically defined as pain, muscle tension, or stiffness localized below the costal margin and above the inferior gluteal folds, with or without leg pain.⁴ Most cases are classified as non-specific LBP because a precise nociceptive source cannot be identified.¹,⁵ LBP may also be categorized as mechanical, arising from the spine or surrounding soft tissues,⁶ or as acute (<6 weeks), subacute (6–12 weeks), or chronic (>12 weeks).⁷ It encompasses axial spinal pain, radicular pain, and referred pain from lumbosacral structures.²
Symptoms
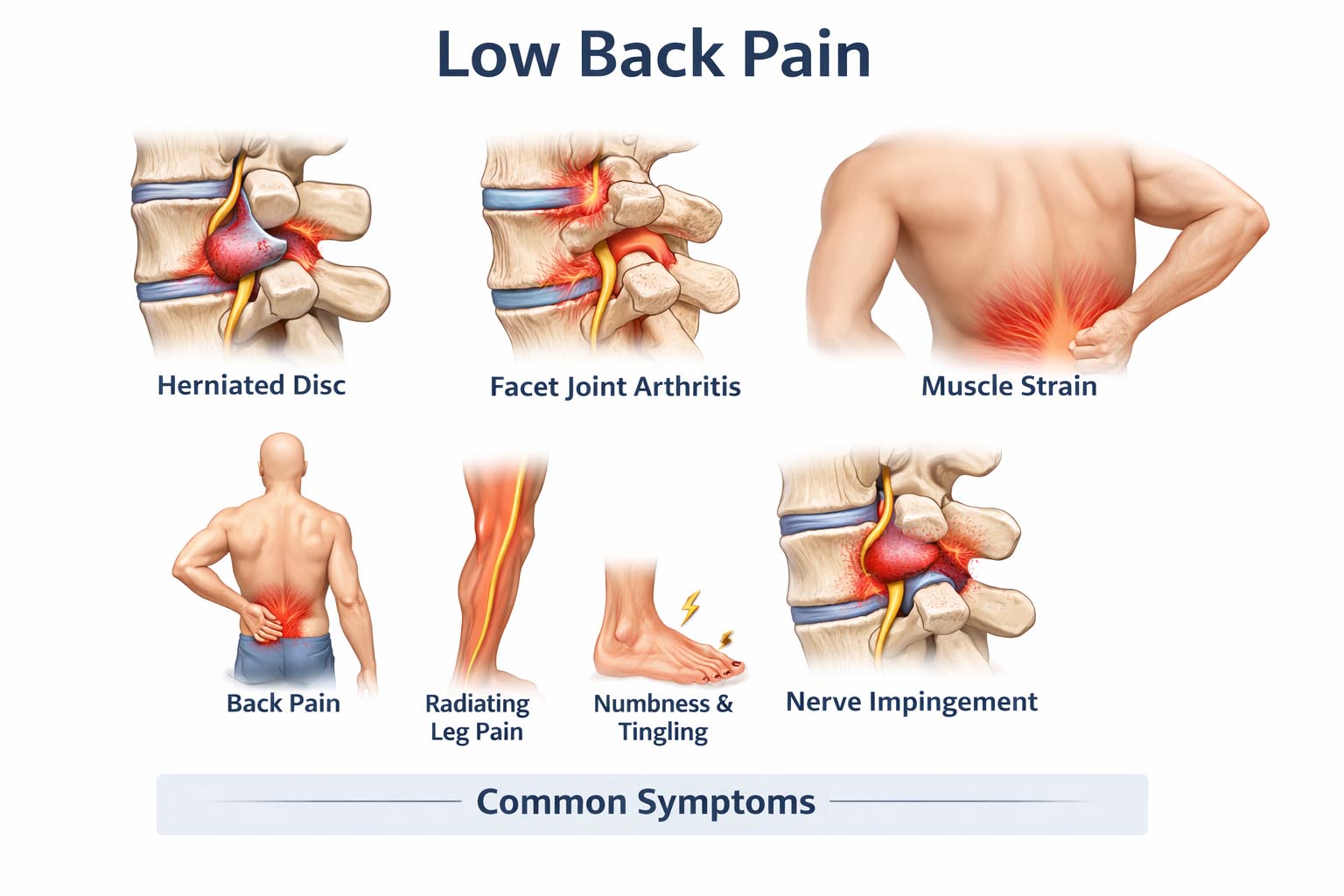
Symptoms vary depending on underlying mechanisms but commonly include:
-
Localized lumbar discomfort, stiffness, or muscle tightness
-
Pain exacerbated by movement, prolonged sitting, or lifting
-
Limited range of motion
-
Occasional pain referral into the buttock or thigh
-
In radiculopathy: sharp, shooting leg pain, dermatomal sensory changes, or weakness²,⁵
Chronic LBP may involve central sensitization, where the nervous system becomes hypersensitive, amplifying pain intensity and reducing tolerance to mechanical load.⁸ Patients may also exhibit psychosocial contributors such as fear-avoidance, maladaptive beliefs, or depression.⁵,⁹
Diagnosis
Diagnosis relies primarily on thorough history-taking and clinical examination, as highlighted by multiple reviews.³,⁵,⁷ Key history features include onset, duration, occupational factors, red flags (trauma, cancer history, infection risk), neurological symptoms, and functional impairment.
Physical examination evaluates posture, gait, range of motion, neurological function, palpation tenderness, and provocative tests.
Most guidelines emphasize not performing routine imaging for acute non-specific LBP unless red flags are present.¹⁰,¹¹ Imaging (X-ray, CT, MRI) is reserved for suspected serious pathology such as fracture, malignancy, infection, inflammatory disease, or cauda equina syndrome.⁵
Mechanical LBP often shows normal imaging or mild age-related degenerative features, which may not correlate with symptoms.⁶
Differential Diagnosis
LBP has a broad differential. Major categories include:
1. Non-specific mechanical LBP (most common)
Due to muscles, ligaments, intervertebral discs, facet joints, or sacroiliac joints.⁶
2. Radicular pain/sciatica
Caused by disc herniation or foraminal stenosis compressing nerve roots.²,⁵
3. Serious spinal pathology (rare)
-
Vertebral fracture
-
Malignancy
-
Infection (discitis, osteomyelitis)
-
Inflammatory spondyloarthropathy⁵,⁷
These account for <1% of cases but require urgent diagnosis.
4. Referred pain
From abdominal, pelvic, or retroperitoneal organs.⁷
5. Lumbar instability
A debated contributor characterized by abnormal segmental motion; prolotherapy has been proposed but evidence remains limited.¹²
6. Central sensitization–driven pain
Often chronic, disproportionate to mechanical findings.⁸
7. Occupational or biomechanical contributors
Heavy lifting, repetitive flexion, manual handling, and vibration exposure increase risk.¹³
Causes
LBP is multifactorial and influenced by biological, mechanical, psychological, and social factors. Key contributors include:
Mechanical/structural factors
-
Age-related disc degeneration
-
Facet arthropathy
-
Muscular strain
-
Ligamentous injury
-
Poor motor control or spinal instability⁶,¹²
Neuropathic mechanisms
Radiculopathy due to disc herniation or stenosis.²
Central sensitization
Longstanding pain leads to increased neural excitability and persistent pain perception even without ongoing tissue injury.⁸
Epidemiologic and lifestyle factors
Sedentary lifestyle, obesity, occupational lifting, smoking, and inadequate physical conditioning increase risk.⁹,¹³
Psychosocial factors
Stress, low job satisfaction, catastrophizing, and depression strongly influence chronicity.⁵,⁹
Most people with new episodes have no identifiable structural pathology, reinforcing that LBP often arises from complex interactions rather than single lesions.¹
Management
Modern management emphasizes multimodal, non-pharmacologic, and patient-centered approaches, as supported across all major guidelines.
1. Education and reassurance
Patients should be informed that acute LBP is common, usually improves within weeks, and that maintaining activity is safe.¹⁰,¹¹ Education reduces fear-avoidance and encourages self-management.
2. Exercise therapy
Exercise is strongly supported for both acute and chronic LBP.⁵,¹⁰ Programs may include:
-
Core stabilization and motor control training
-
Aerobic exercise
-
Flexibility and strengthening work
-
Loaded exercise programs (e.g., deadlift-based rehabilitation) show promising results in selected patients¹⁴
3. Physical therapy and manual approaches
Mechanical therapy principles such as the McKenzie method may reduce symptoms.⁶
Manual therapy, massage, and spinal mobilization can provide adjunctive benefit.
4. Psychosocial and behavioral interventions
Cognitive behavioral therapy and pain-coping strategies reduce disability, especially in chronic or centrally sensitized pain.⁵,⁸
5. Pharmacological measures
Used sparingly:
-
NSAIDs for short-term relief
-
Avoid routine opioids
-
Adjuncts only when necessary and in chronic cases with neuropathic features⁵
6. Interventional therapies
Epidural injections may help selected radicular pain patients.
Prolotherapy and other regenerative approaches remain investigational.¹²
7. Surgical referral
Reserved for:
-
Cauda equina syndrome
-
Major neurological deficits
-
Severe refractory radiculopathy with structural compression
Routine surgery for non-specific pain is not recommended.⁵
8. Mechanism-based and multidisciplinary care
Recent perspectives highlight shifting toward mechanism-based management, integrating biological, mechanical, and psychosocial mechanisms to tailor individualized care.¹⁵
Prognosis
Most patients with acute LBP improve significantly within the first 4–6 weeks.¹⁷ However, recurrence is common, and up to 40% may develop persistent symptoms.⁹ Risk factors for chronicity include high initial pain, psychosocial distress, maladaptive beliefs, central sensitization, and occupational strain.⁵,⁸
Chronic LBP tends to fluctuate rather than follow a linear course. While pain may persist, disability can be minimized through consistent exercise, self-management, and modification of psychosocial risk factors.
Overall, although LBP is highly prevalent, the prognosis is favorable for most individuals, especially with active and guideline-concordant management.
References
-
Hartvigsen J, Hancock MJ, Kongsted A, Louw Q, Ferreira ML, Genevay S, Hoy D, Karppinen J, Pransky G, Sieper J, Smeets RJ, Underwood M; Lancet Low Back Pain Series Working Group. What low back pain is and why we need to pay attention. Lancet. 2018 Jun 9;391(10137):2356-2367. doi: 10.1016/S0140-6736(18)30480-X. Epub 2018 Mar 21.
-
Urits I, Burshtein A, Sharma M, Testa L, Gold PA, Orhurhu V, Viswanath O, Jones MR, Sidransky MA, Spektor B, Kaye AD. Low Back Pain: A Comprehensive Review: Pathophysiology, Diagnosis, and Treatment. Curr Pain Headache Rep. 2019 Mar 11;23(3):23. doi: 10.1007/s11916-019-0757-1.
-
Kabeer AS, Osmani HT, Patel J, Robinson P, Ahmed N. The adult with low back pain: causes, diagnosis, imaging features and management. Br J Hosp Med (Lond). 2023 Oct 2;84(10):1-9. doi: 10.12968/hmed.2023.0063. Epub 2023 Oct 25.
-
Will JS, Bury DC, Miller JA. Mechanical Low Back Pain. Am Fam Physician. 2018 Oct 1;98(7):421-428.
-
Chou R. Low Back Pain. Ann Intern Med. 2021 Aug;174(8):ITC113-ITC128. doi: 10.7326/AITC202108170. Epub 2021 Aug 10.
-
Balagué F, Mannion AF, Pellisé F, Cedraschi C. Non-specific low back pain. Lancet. 2012 Feb 4;379(9814):482-491. doi: 10.1016/S0140-6736(11)60610-7. Epub 2011 Oct 6.
-
Patrick N, Emanski E, Knaub MA. Acute and chronic low back pain. Med Clin North Am. 2014 Jul;98(4):777-789. doi: 10.1016/j.mcna.2014.03.005.
-
Koes BW, van Tulder MW, Thomas S. Diagnosis and treatment of low back pain. BMJ. 2006 Jun 17;332(7555):1430-1434. doi: 10.1136/bmj.332.7555.1430.
-
Hoy D, Brooks P, Blyth F, Buchbinder R. The epidemiology of low back pain. Best Pract Res Clin Rheumatol. 2010 Dec;24(6):769-781. doi: 10.1016/j.berh.2010.10.002.
-
Meucci RD, Fassa AG, Faria NM. Prevalence of chronic low back pain: systematic review. Rev Saude Publica. 2015;49:1. doi: 10.1590/S0034-8910.2015049005874. Epub 2015 Oct 20.
-
Borenstein DG, Balagué F. Low Back Pain in Adolescent and Geriatric Populations. Rheum Dis Clin North Am. 2021 May;47(2):149-163. doi: 10.1016/j.rdc.2020.12.001. Epub 2021 Mar 12.
-
Violante FS, Mattioli S, Bonfiglioli R. Low-back pain. Handb Clin Neurol. 2015;131:397-410. doi: 10.1016/B978-0-444-62627-1.00020-2.
-
Hauser RA, Matias D, Woznica D, Rawlings B, Woldin BA. Lumbar instability as an etiology of low back pain and its treatment by prolotherapy: A review. J Back Musculoskelet Rehabil. 2022;35(4):701-712. doi: 10.3233/BMR-210097.
-
Fischer SC, Calley DQ, Hollman JH. Effect of an Exercise Program That Includes Deadlifts on Low Back Pain. J Sport Rehabil. 2021 Feb 24;30(4):672-675. doi: 10.1123/jsr.2020-0324.
-
Sanzarello I, Merlini L, Rosa MA, Perrone M, Frugiuele J, Borghi R, Faldini C. Central sensitization in chronic low back pain: A narrative review. J Back Musculoskelet Rehabil. 2016 Nov 21;29(4):625-633. doi: 10.3233/BMR-160685.
-
Golob AL, Wipf JE. Low back pain. Med Clin North Am. 2014 May;98(3):405-428. doi: 10.1016/j.mcna.2014.01.003. Epub 2014 Mar 22.
-
Tavee JO, Levin KH. Low Back Pain. Continuum (Minneap Minn). 2017 Apr;23(2):467-486. doi: 10.1212/CON.0000000000000449.
-
Bernstein IA, Malik Q, Carville S, Ward S. Low back pain and sciatica: summary of NICE guidance. BMJ. 2017 Jan 6;356:i6748. doi: 10.1136/bmj.i6748.
-
Earwood JS, Doles NA, Russell RS. Acute Low Back Pain: Diagnosis and Management. Am Fam Physician. 2025 Nov;112(5):526-536.
-
Mousavi SJ, van Dieën JH, Anderson DE. Low back pain: Moving toward mechanism-based management. Clin Biomech (Bristol). 2019 Jan;61:190-191. doi: 10.1016/j.clinbiomech.2018.12.010. Epub 2018 Dec 11.