Prevalence and Overview
Diffuse idiopathic skeletal hyperostosis (DISH) is a systemic, non-inflammatory condition characterized by abnormal ossification of ligaments and entheses, particularly along the anterolateral aspect of the spine 1. It is most commonly identified in older adults and has been reported to affect up to 32.5% of certain populations, depending on diagnostic criteria and imaging methods 3. The condition is more prevalent in males and is frequently associated with metabolic disorders such as obesity, type 2 diabetes mellitus, and hyperinsulinemia 4. Historical and bioarchaeological data suggest that DISH has been present for centuries, with prevalence influenced by dietary and lifestyle factors 12. Despite its relatively high prevalence, DISH is often underdiagnosed due to its slow progression and frequently asymptomatic early stages 20.
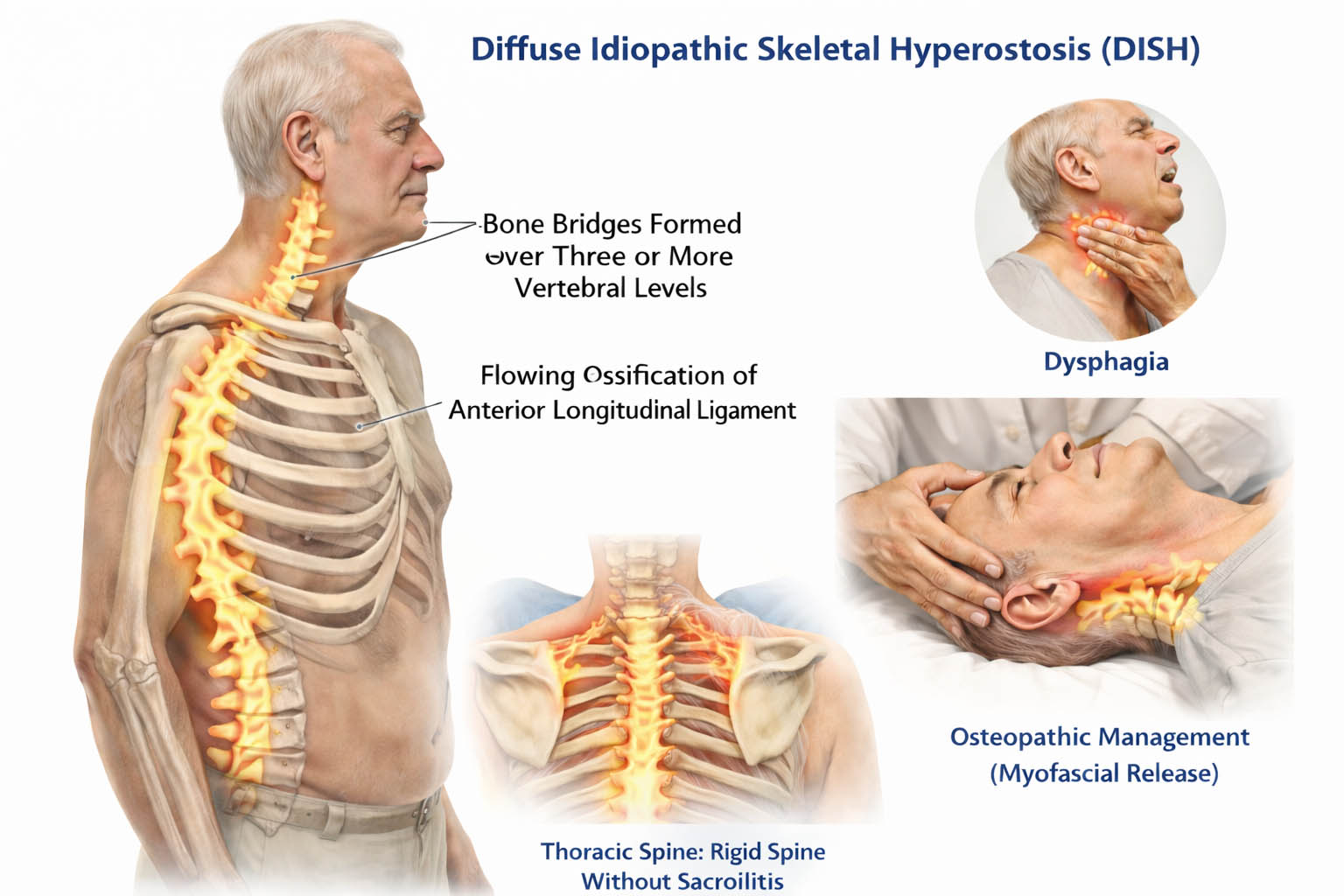
Etiology
The etiology of DISH remains incompletely understood, though it is widely regarded as a multifactorial condition involving metabolic, genetic, and mechanical factors. Current evidence suggests that DISH is associated with increased osteoblastic activity at entheses, resulting in excessive bone formation 4. Genetic studies have identified potential hereditary components, although no single gene has been definitively implicated 13. Environmental and metabolic influences, particularly insulin-like growth factors and hyperinsulinemia, are believed to stimulate new bone formation 1. Mechanical stress may further contribute by promoting ossification at sites of repetitive strain 20.
Although DISH has traditionally been considered a non-inflammatory condition, emerging evidence suggests a possible inflammatory component, particularly in early disease stages 4. This has led to ongoing debate regarding its classification and its distinction from other spondyloarthropathies. The condition is clearly differentiated from ankylosing spondylitis by the absence of sacroiliac joint erosion and by its characteristic flowing ossifications rather than syndesmophytes 5.
Signs and Symptoms
Many individuals with DISH remain asymptomatic, particularly in early stages. When symptoms occur, they are typically related to stiffness and reduced spinal mobility rather than pain. Patients often report progressive limitation in spinal flexibility, especially in the thoracic region 8. Pain, when present, is usually mild and mechanical in nature, arising from altered biomechanics and secondary degenerative changes 11.
In advanced cases, large anterior cervical osteophytes may lead to dysphagia, hoarseness, or even airway compromise due to compression of adjacent structures 6. Respiratory symptoms have also been reported in severe cases where ossification affects thoracic mobility or airway structures 16. Neurological symptoms are uncommon but may occur if spinal cord or nerve roots are compressed. Because DISH affects multiple entheses, patients may also experience peripheral manifestations such as heel pain or tendon stiffness 2.
Diagnosis
Diagnosis of DISH is primarily radiographic. Classic criteria include the presence of flowing ossification along the anterolateral aspect of at least three or more contiguous vertebral bodies with preservation of intervertebral disc height and absence of sacroiliac joint degeneration 1. Conventional radiography remains the primary imaging modality, although computed tomography (CT) and magnetic resonance imaging (MRI) can provide additional detail, particularly in complex or symptomatic cases 7.
Differentiating DISH from ankylosing spondylitis and other spondyloarthropathies is critical. Unlike inflammatory disorders, DISH does not typically present with elevated inflammatory markers or significant morning stiffness. However, overlap cases have been reported, complicating diagnosis and management 9. Clinical assessment should also include evaluation of metabolic risk factors, which are frequently associated with the condition.
Management and Treatment
Management of DISH is primarily conservative and focuses on symptom control and prevention of complications. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be used to relieve discomfort, although inflammation is not a primary driver of the disease 8. Physical therapy plays a central role, emphasizing maintenance of spinal mobility, postural correction, and strengthening of supporting musculature.
In cases where large osteophytes cause significant dysphagia or airway obstruction, surgical intervention may be necessary. Surgical removal of anterior cervical osteophytes has been shown to improve swallowing function and airway patency 17. However, recurrence is possible, and surgery is generally reserved for severe or refractory cases. Management of associated metabolic conditions such as diabetes and obesity is also important, as these factors may contribute to disease progression 3.
Role of Osteopathic Management
Osteopathic management can play a valuable supportive role in patients with DISH by addressing secondary biomechanical dysfunction and improving overall mobility. Although osteopathic manipulative treatment (OMT) does not alter the underlying ossification process, it can reduce compensatory strain patterns, improve joint function, and alleviate discomfort associated with stiffness.
Techniques such as myofascial release, muscle energy, and soft tissue mobilization may help improve flexibility in surrounding musculature and enhance functional movement. Gentle articulation techniques may assist in maintaining mobility in non-ossified segments of the spine. High-velocity low-amplitude (HVLA) techniques are generally used cautiously due to the rigidity of the spine and potential fracture risk. Osteopathic care also emphasizes posture, breathing mechanics, and patient education, which are essential in minimizing functional limitations and improving quality of life.
Prognosis and Prevention
DISH is typically a slowly progressive condition with a generally favorable prognosis in terms of life expectancy. However, functional limitations may increase over time due to progressive spinal rigidity. Early diagnosis and proactive management can help preserve mobility and reduce complications. Preventive strategies focus on addressing modifiable risk factors such as obesity, metabolic syndrome, and sedentary lifestyle 1.
Regular exercise, maintenance of spinal flexibility, and monitoring of metabolic health are key components of long-term management. While the condition cannot be fully prevented, early recognition and intervention can significantly improve functional outcomes and reduce the impact on daily life.
References
8. Graham P. Diffuse Idiopathic Skeletal Hyperostosis. Orthop Nurs. 2022;41(3):237-239.
10. Rothschild BM. Diffuse idiopathic skeletal hyperostosis. Compr Ther. 1988;14(2):65-69.
11. Utsinger PD. Diffuse idiopathic skeletal hyperostosis. Clin Rheum Dis. 1985;11(2):325-351.
13. Kato H, Braddock DT, Ito N. Genetics of DISH. Curr Osteoporos Rep. 2023;21(5):552-566.
15. Gilio M, et al. DISH in an HLA-B27-positive subject. J Clin Rheumatol. 2019;25(6):e94-e98.
16. Dell'Era V, et al. Respiratory presentation of DISH. Cranio. 2022;40(1):88-91.
17. Bunmaprasert T, et al. Surgical management of DISH causing dysphagia. J Orthop Surg. 2021;29(3).
18. Colina M, et al. Diffuse idiopathic skeletal hyperostosis. Reumatismo. 2006;58(2):104-111.
19. De Mattia G, et al. One year in review 2025. Clin Exp Rheumatol. 2025;43(7):1195-1203.