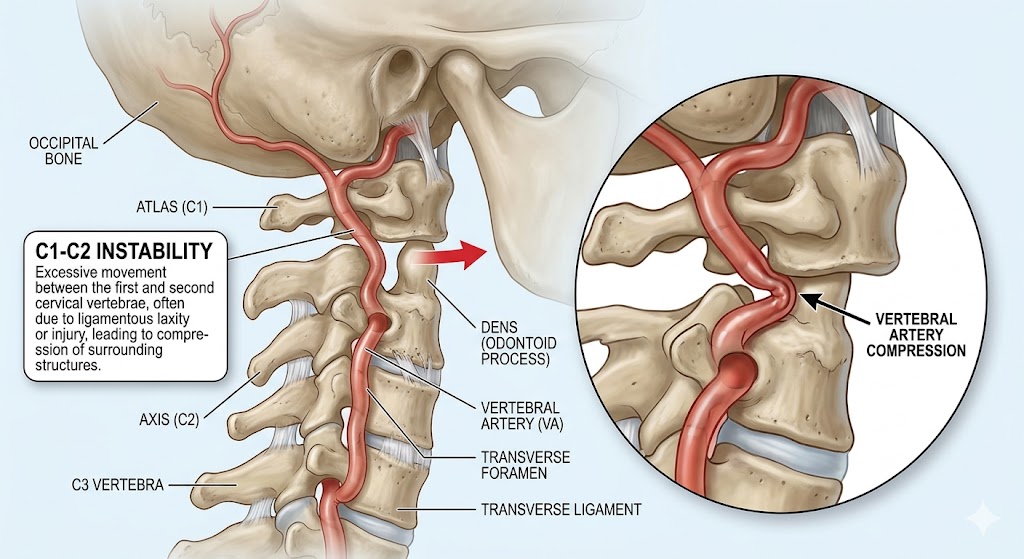
C1–C2 instability refers to excessive or pathological movement between the atlas and axis, two vertebrae responsible for more than half of cervical rotation. Instability may lead to neck pain, neurological deficits, spinal cord compression, or life-threatening complications. With increasing availability of advanced imaging and surgical innovations, the understanding and management of atlantoaxial instability have expanded significantly in recent years.
Prevalence
C1–C2 instability is relatively uncommon in the general population but occurs more frequently in individuals with predisposing disorders. It presents notably in patients with inflammatory arthropathies such as psoriatic arthritis, where atlantoaxial arthritis and ligament degeneration may develop over time2. Among individuals with congenital anomalies, including os odontoideum, instability may be found even in the absence of symptoms but carries substantial long-term risk10. Pediatric patients with skeletal dysplasias such as Morquio syndrome constitute another vulnerable population, often developing early instability with potential compressive myelopathy8. Traumatic instability remains a significant cause across all age groups, particularly following odontoid fractures or high-energy cervical trauma.
Etiology
Etiologies of C1–C2 instability include trauma, inflammation, congenital malformations, infection, and degenerative changes. Traumatic injury remains a common cause, with odontoid fractures and transverse ligament disruption being key contributors. Degenerative or inflammatory conditions such as psoriatic arthritis show a predilection for upper cervical involvement and may lead to progressive ligamentous compromise or erosive changes within the atlantoaxial joint2. Congenital anomalies such as os odontoideum create inherent mechanical vulnerability, contributing to chronic instability or sudden deterioration10. Infectious etiologies such as Grisel’s syndrome, involving inflammatory laxity of peri-odontoid structures following upper respiratory infections, represent another recognized cause11. In hereditary conditions such as Morquio syndrome, ligamentous hyperlaxity and malformed odontoid structures significantly increase the risk of early instability8.
Signs and Symptoms
Symptoms of C1–C2 instability vary depending on the severity of mechanical disruption and the presence of neurological involvement. Patients may present with suboccipital pain, neck stiffness, rotational limitations, or a sense of head heaviness. Neurological signs include limb numbness, weakness, gait disturbance, and in severe cases, bladder or bowel dysfunction due to spinal cord compression. In os odontoideum, patients may be asymptomatic initially but may develop acute symptoms after minor trauma10. Pediatric patients with Morquio syndrome often present with early progressive myelopathy arising from instability8. When infection-related, such as in Grisel’s syndrome, torticollis and painful restricted motion are characteristic clinical features11.
Diagnosis
Diagnosis requires a combination of clinical assessment and imaging. Radiographic evaluation includes open-mouth odontoid views, lateral radiographs, and dynamic flexion-extension studies to assess abnormal motion. CT imaging is essential for bony anatomy, while MRI evaluates ligament integrity, inflammation, and cord compression. Radiographic indices, such as the C1–C2 overlap measurement, have been validated in veterinary models and help refine diagnostic thresholds; a negative overlap value strongly predicts instability7. In cases of congenital anomalies, MRI plays a central role in determining whether surveillance or surgical stabilization is indicated10.
Management
Management is determined by symptom severity, degree of instability, and neurological risk. Conservative management may be suitable for mild cases or asymptomatic congenital conditions, involving immobilization, inflammation control, and activity modification10. When instability is pronounced or neurological compromise is present, surgical stabilization becomes necessary.
Posterior C1–C2 fixation is the cornerstone of operative management. Techniques include transarticular screws and screw-rod constructs, which can be performed using fluoroscopy-assisted free-hand methods or 3D-navigation systems3. Historically, wiring techniques were used, but modern screw-based systems offer superior biomechanical stability9. Recent biomechanical research suggests that transverse connectors may enhance construct rigidity under certain conditions, although their necessity remains debated14. Alternative approaches such as C1–C2 claw fixation provide a screw-less option in select patients13. Novel techniques, including C1–C2 arthroplasty, have emerged as experimental strategies aimed at preserving motion while restoring stability1.
Osteopathic Management
Osteopathic treatment supports biomechanical balance and symptom reduction but must be approached with caution. Direct manipulation of the upper cervical spine is contraindicated when instability is suspected or confirmed. Instead, osteopathic care focuses on adjacent regions such as the thoracic spine, rib cage, diaphragm, and pelvis to reduce compensatory strain at the C1–C2 segment. Gentle soft-tissue techniques, myofascial release, balanced ligamentous tension approaches, and muscle-energy techniques may improve functional mobility and reduce symptom severity without stressing the unstable region. Through optimizing whole-spine biomechanics, osteopathic treatment complements medical or surgical intervention.
Prognosis
The prognosis varies widely depending on the underlying etiology and timeliness of treatment. Early stabilization in high-risk congenital or inflammatory conditions can prevent irreversible neurological injury8. Surgical fixation has demonstrated high fusion success rates and sustained symptom improvement across multiple patient groups16. Delayed treatment or untreated instability can lead to progressive myelopathy, chronic pain, or catastrophic spinal cord injury.
Prevention
Prevention strategies include early detection of congenital anomalies such as os odontoideum, surveillance in high-risk pediatric populations, and aggressive management of inflammatory arthropathies to minimize joint destruction10. Avoiding high-risk trauma, addressing infection promptly to prevent Grisel’s syndrome, and promoting safe spinal biomechanics also reduce the likelihood of instability developing or progressing.