Cervical facet dysfunction is a prevalent yet frequently underdiagnosed contributor to chronic neck pain, stiffness, and movement impairment. The cervical facet joints are synovial articulations that guide and limit spinal motion while sharing load-bearing responsibilities with the intervertebral discs. When these joints undergo injury, degeneration, or altered biomechanics, they become potent generators of nociception and functional impairment. Osteopathy, with its emphasis on structural–functional relationships and manual techniques aimed at restoring mobility and reducing neuromuscular imbalance, offers a significant therapeutic approach to managing cervical facet dysfunction. Evidence from biomechanical, clinical, and degenerative spine research underscores the relevance of osteopathic management in this condition.
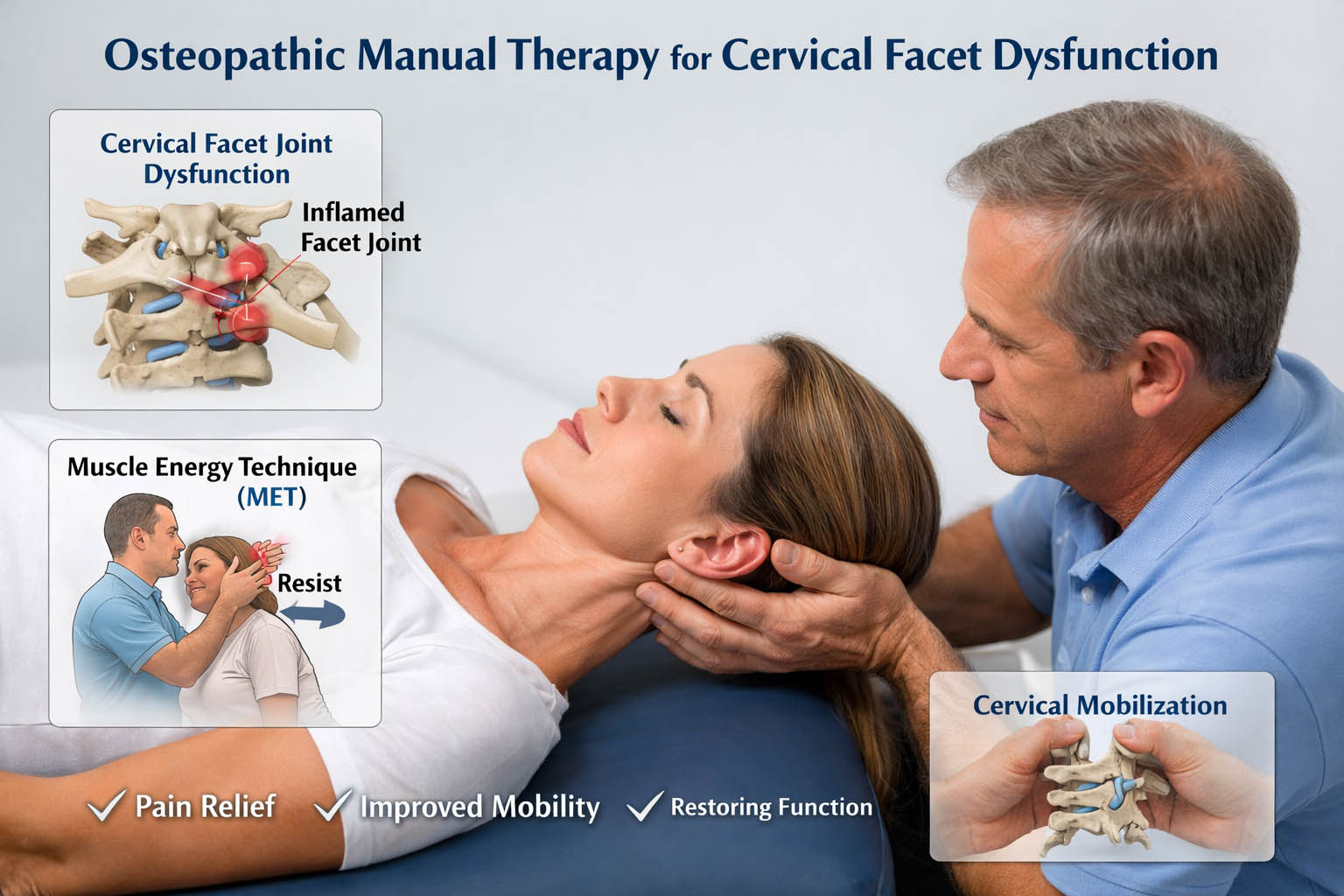
Cervical Facet Joint Biomechanics and Dysfunction
Healthy facet joint function depends on normal load distribution, joint capsule integrity, and coordinated motion across cervical segments. Jaumard et al. demonstrated that facet joint mechanotransduction maintains spinal health under physiological loading, but mechanical disruption—whether traumatic, degenerative, or postsurgical—alters joint mechanics and increases susceptibility to pain and dysfunction [1]. Excessive capsular strain, asymmetric loading, and segmental instability provoke inflammatory cascades linked directly to nociceptive signaling within the facet joint.
Biomechanical studies consistently show that facet joints bear significant loads during extension and rotation, the very movements commonly restricted in patients with cervical pain syndromes. Ansaripour et al. noted that pathological conditions such as degeneration increase facet joint loads and reduce segmental range of motion, further perpetuating dysfunction [16]. Crawford and colleagues found that even unilateral facet injury drastically alters cervical kinematics, compromising stability and promoting abnormal motion patterns across segments [9].
These findings align strongly with osteopathic principles, which emphasize early identification of motion restriction, asymmetry, and tissue texture changes—key features of the ARTS assessment framework commonly used in osteopathic care.
Degeneration, Facet Tropism, and Neck Pain
Degenerative changes of the facet joints constitute a major cause of chronic neck pain. Gellhorn et al. highlighted that facet osteoarthritis represents a whole-joint failure, involving cartilage erosion, capsular thickening, inflammatory changes, and subchondral remodeling [2]. These degenerative changes compromise joint motion and heighten nociceptor activation, explaining why many patients experience persistent axial neck pain.
Facet tropism—the asymmetry of facet joint orientation between left and right sides—further contributes to uneven load distribution. Multiple studies [5, 8, 10, 11] show that facet tropism is significantly associated with cervical degenerative disorders, disc herniation, motor dysfunction, and increased facet joint stress. The presence of tropism exacerbates segmental imbalance and predisposes patients to unilateral pain patterns, muscular guarding, and reduced proprioception.
Osteopathy is uniquely suited to address asymmetry-driven dysfunction. Through hands-on assessment and corrective manual procedures, osteopathic practitioners work to improve symmetry of motion, reduce fascial and muscular tension, and restore normal segmental biomechanics.
Relationship Between Cervical Facet Dysfunction and Neurological Conditions
Degenerative changes of the cervical facets also contribute to more serious neurological disorders. In cervical spondylotic myelopathy, degenerative processes involving discs, vertebral bodies, ligaments, and facets collectively encroach on the spinal canal, causing myelopathic symptoms [6, 19]. Walraevens et al. demonstrated that facet degeneration is quantifiable and strongly correlated with progressive cervical spine pathology [14].
Similarly, ankylosing spondylitis and rheumatoid arthritis lead to facet ankylosis, which alters spinal stiffness and motion patterns, compounding pain and disability [17, 18]. While osteopathy does not reverse structural ankylosis, gentle mobility techniques and soft-tissue approaches can reduce compensatory strain at adjacent mobile segments.
Adjacent segment disease (ASD) following surgical interventions such as fusion or artificial disc replacement is also partly explained by altered facet loading. Virk et al. showed that altered biomechanics predispose adjacent levels to degeneration [4], while Li et al. found that facet tropism increases facet joint pressure following artificial disc replacement [11]. These findings underscore the importance of maintaining optimal spinal motion and balance—core goals within osteopathic treatment.
Pain Mechanisms in Facet-Mediated Disorders
The facet joint capsule is richly innervated with nociceptive fibers capable of generating significant pain when mechanically stressed. Sperry et al. described how mechanical strain triggers molecular responses that amplify inflammation and nociception within the facet joint [20]. This explains why patients often present with deep, localized axial pain that worsens with extension or rotation.
Radiofrequency neurolysis is frequently used to denervate painful facet joints [7], demonstrating the recognition of facets as significant pain contributors. However, osteopathic approaches aim to address the underlying biomechanical dysfunction rather than focusing solely on neural interruption.
Evidence Supporting Osteopathic Treatment
Osteopathic techniques have shown promising outcomes in cervical facet-related conditions. A clinical study by Sezerel and Yüksel compared osteopathic Muscle Energy Technique (MET) with conventional cervical mobilization and found that both were effective in reducing pain, disability, and proprioceptive deficits in cervical spondylosis [3]. MET emphasizes active patient participation to restore joint mobility, reduce hypertonicity, and normalize neuromuscular control—mechanisms directly relevant to facet dysfunction.
Osteopathic manual therapy also aligns with the broader understanding of facet joint pathophysiology described by O’Leary et al., who emphasized the potential for regeneration and the importance of maintaining healthy mechanics in preventing joint degeneration [13].
Why Osteopathy Matters in Cervical Facet Dysfunction
1. Restores Segmental Motion:
Facet dysfunction manifests primarily as motion restriction. Osteopathic mobilization and MET techniques directly improve segmental rotation, sidebending, and extension.
2. Reduces Joint Capsule Strain:
By normalizing muscle tension and improving posture, osteopathy lowers mechanical load on sensitized facet capsules.
3. Modulates Pain Through Neuromuscular Pathways:
Manual therapy reduces nociceptive input and improves proprioception, key components in chronic facet-mediated neck pain.
4. Addresses Whole-Spine Biomechanics:
Osteopathy considers thoracic and lumbar compensation patterns, essential because altered global posture increases cervical facet loading.
5. Complements Medical and Interventional Care:
Osteopathy offers conservative management that can delay or reduce the need for injections, radiofrequency ablation, or surgery.
Conclusion
The cumulative body of research supports the significant role that cervical facet joints play in neck pain, degeneration, and spinal dysfunction. Osteopathy, through its holistic, biomechanical, and patient-centered approach, offers effective strategies to reduce facet joint stress, restore proper mobility, and alleviate pain. By integrating osteopathic principles with current evidence on facet joint mechanics and pathology, clinicians can provide comprehensive care that addresses both symptoms and underlying dysfunction.
References
- Jaumard NV, Welch WC, Winkelstein BA. J Biomech Eng. 2011;133(7):071010.
- Gellhorn AC, Katz JN, Suri P. Nat Rev Rheumatol. 2013;9(4):216-24.
- Sezerel B, Yüksel İ. Med Sci Monit. 2024;30:e945149.
- Virk SS, Niedermeier S, Yu E, Khan SN. Orthopedics. 2014;37(8):547-55.
- Garg K, Aggarwal A. World Neurosurg. 2021;147:47-65.
- Tracy JA, Bartleson JD. Neurologist. 2010;16(3):176-87.
- Golovac S. Neuroimaging Clin N Am. 2010;20(2):203-14.
- Wang Y, Chen G, Lin J, et al. Spine (Phila Pa 1976). 2021;46(5):E310-E317.
- Crawford NR, Duggal N, Chamberlain RH, et al. Spine (Phila Pa 1976). 2002;27(17):1858-64.
- Ji Y, Chen K, Gu S, et al. Eur Spine J. 2025;34(8):3196-3204.
- Li J, Deng Y, Zhang J, et al. BMC Musculoskelet Disord. 2024;25(1):839.
- Aydogan M, Enercan M, Hamzaoglu A, Alanay A. Spine (Phila Pa 1976). 2012;37(5):E335-41.
- O'Leary SA, Paschos NK, Link JM, et al. Annu Rev Biomed Eng. 2018;20:145-70.
- Walraevens J, Liu B, Meersschaert J, et al. Eur Spine J. 2009;18(3):358-69.
- Feng G, Hong Y, Li L, et al. Spine (Phila Pa 1976). 2012;37(25):2082-8.
- Ansaripour H, Ferguson SJ, Flohr M. J Biomech Eng. 2022;144(10):100801.
- Iizuka H, Iizuka Y, Okamura K, et al. Mod Rheumatol. 2017;27(5):801-5.
- Maas F, Spoorenberg A, Brouwer E, et al. Semin Arthritis Rheum. 2017;46(5):562-8.
- Shedid D, Benzel EC. Neurosurgery. 2007;60(S1):S7-13.
- Sperry MM, Ita ME, Kartha S, et al. J Biomech Eng. 2017;139(2):021003.