Introduction
Neck pain is one of the most common musculoskeletal complaints worldwide and ranks as the fourth leading cause of disability.¹ Its annual prevalence surpasses 30%, affecting people of all ages and lifestyles. Although neck pain can originate from muscles, discs, ligaments, and nerves, a substantial body of research now identifies the cervical facet joints—also known as zygapophysial joints—as a major contributor to both acute and chronic neck pain. Appreciating how these joints create pain, how clinicians accurately diagnose their involvement, and what treatments have proven effective is essential for guiding patients toward meaningful and lasting relief.
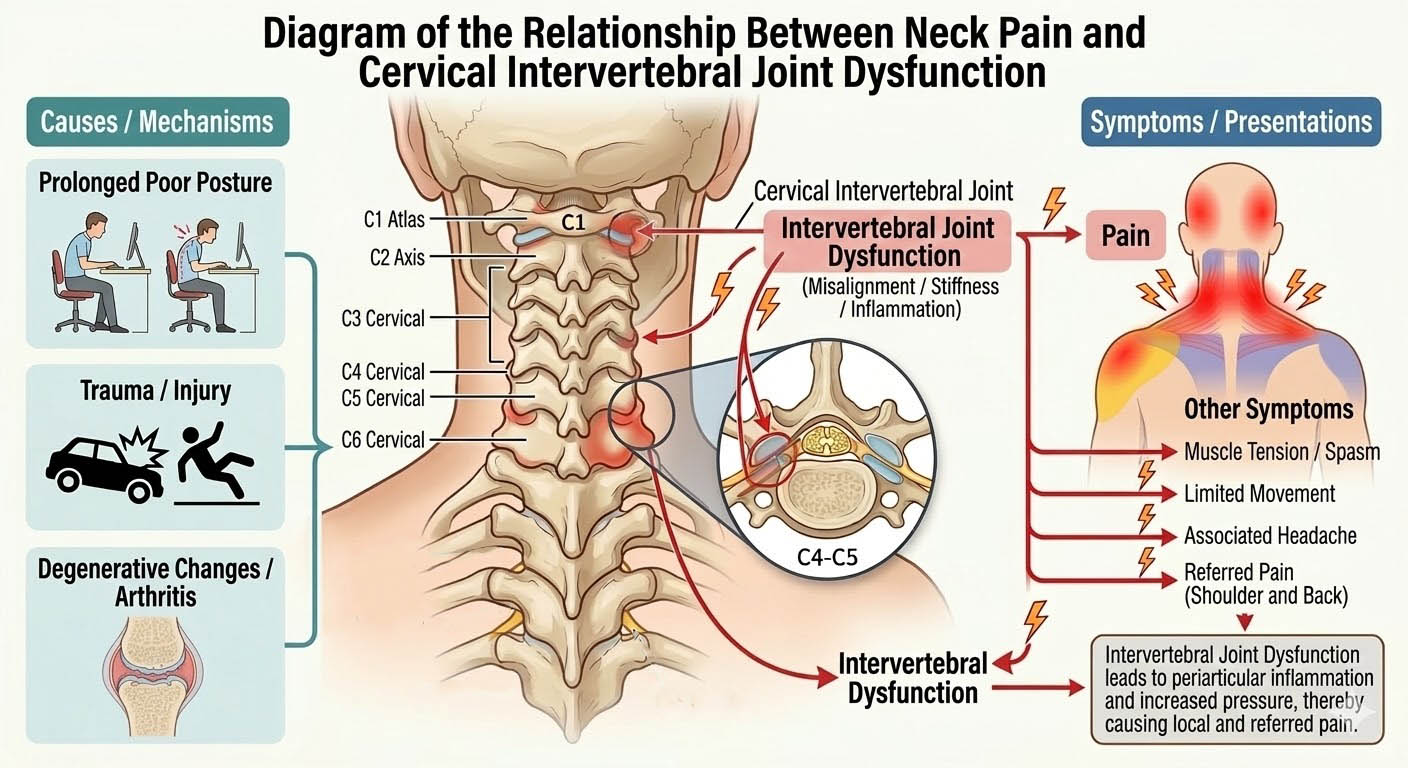
Anatomy and Function of the Cervical Facet Joints
Cervical facet joints are paired synovial joints located between each vertebra from C2–C3 down to C7–T1. Each joint is enclosed by a capsule, lined with synovium, and richly innervated by the medial branches of the dorsal rami. This neural supply explains why irritation of these joints can cause significant discomfort and refer pain to the head, neck, shoulder regions, or upper thoracic spine. Early clinical descriptions by Bogduk emphasized that any structure innervated by cervical spinal nerves may produce neck pain, but the facet joints and intervertebral discs remain among the most common sources [6].
Prevalence of Facet-Mediated Neck Pain
Research suggests that approximately 25% to 55% of chronic neck pain cases may arise from the cervical facet joints. This high prevalence has led to a considerable increase in the use of diagnostic and therapeutic facet joint interventions worldwide. A 2022 international multispecialty guideline noted that the use of these procedures has expanded rapidly in the past two decades, reflecting both clinical recognition and growing evidence supporting their effectiveness [2].
Mechanisms of Cervical Facet Joint Pain
Degeneration and Osteoarthritis
Age-related degeneration of the facet joints is one of the most common causes of chronic neck pain. Over time, these joints undergo biochemical and structural changes, including cartilage thinning, osteophyte formation, capsular thickening, and synovial inflammation. These degenerative processes sensitize pain receptors within the joint and can result in persistent stiffness, localized pain, and restricted mobility. [5] In older adults, facet joint osteoarthritis is especially prevalent and often contributes significantly to cervical spine symptoms.
Trauma and Whiplash Injury
Whiplash injuries, most often resulting from motor vehicle collisions, represent another major cause of cervical facet pain. Biomechanical studies show that rapid acceleration and deceleration forces place substantial strain on the facet joint capsules. When these ligaments stretch beyond their physiological limits, they activate nociceptors and can produce both immediate and long-term pain. [4] After whiplash, the C2–C3 and C5–C6 joints are particularly vulnerable to injury. Many patients develop upper cervical pain, headaches, and loss of rotation—patterns consistent with facet-mediated trauma.
Inflammation and Capsular Irritation
Inflammation within the facet joint capsule can occur following degeneration, trauma, or repetitive mechanical stress. This inflammation increases joint pressure and irritates the richly innervated joint capsule. Patients frequently experience pain that intensifies with extension, rotation, or lateral bending. Anti-inflammatory treatments such as corticosteroid injections may provide symptom improvement, particularly in acute or subacute cases. [14]
Clinical Presentation and Symptom Patterns
Cervical facet joint dysfunction typically presents as axial neck pain without neurological symptoms. The pain often worsens with activities that load or compress the facet joints, including backward bending and rotation. Patients may describe stiffness, morning discomfort, and limited range of motion. Because the facet joints share nerve supply with adjacent regions, the pain may radiate into the occipital area, shoulders, or scapular region.
Certain rare conditions highlight the complex neural relationships within the upper cervical spine. Neck-Tongue Syndrome, for instance, involves sudden neck pain combined with transient tongue paresthesia triggered by rapid rotation of the head. This condition is believed to involve upper cervical facet joint irritation and the unique neural connections between the upper cervical spine and the hypoglossal pathways. [10]
Diagnosis of Cervical Facet Joint Pain
Accurately diagnosing facet-mediated pain remains a clinical challenge. Although imaging techniques such as X-ray, CT, and MRI can reveal degenerative changes, these findings do not necessarily correlate with symptoms. Degeneration is extremely common even in asymptomatic individuals. Consequently, the literature consistently concludes that facet joint pain cannot be diagnosed based solely on imaging. [1, 9]
The most reliable diagnostic method is the medial branch block. This procedure involves injecting a small amount of local anesthetic around the medial branch nerves that supply the facet joints. If the patient experiences a substantial reduction in pain, the test confirms the facet joint as the primary pain generator. Numerous reviews and guidelines emphasize that diagnostic blocks are the gold standard for identifying cervical facet-mediated pain. [3, 9, 13]
Evidence-Based Treatment Options
Exercise and Physical Rehabilitation
Exercise therapy forms the foundation of conservative management for most types of neck pain, including facet-related pain. Although exercise alone may not specifically target the irritated facet joint, it plays an important role in improving cervical mobility, posture, and muscular endurance. Such improvements can reduce overall pain and support the spine’s ability to tolerate daily activities. [1]
Corticosteroid Injections
For patients who do not fully respond to conservative care, intra-articular corticosteroid injections may help reduce inflammation within the facet joint. Evidence suggests that these injections can be particularly helpful for individuals experiencing whiplash-related facet pain. [14] However, the long-term effectiveness of corticosteroids remains uncertain. A 2024 Cochrane review concluded that although corticosteroid facet injections may provide temporary relief, their sustained benefits are unclear. [7]
Radiofrequency Ablation
Radiofrequency ablation (RFA) of the medial branch nerves is one of the most effective long-term treatments for confirmed facet-mediated neck pain. By temporarily denervating the nerves that transmit pain from the joint, RFA can substantially reduce symptoms for six to eighteen months or longer. Systematic reviews demonstrate that RFA offers clinically meaningful reductions in pain and disability, particularly in patients who have responded positively to diagnostic medial branch blocks. [8] Updated international guidelines strongly recommend RFA for chronic facet joint pain when appropriate diagnostic criteria are met. [2]
Interventional and Rehabilitative Integration
In addition to injections and RFA, other interventional options include therapeutic medial branch blocks and regenerative procedures, although evidence for the latter remains limited. Regardless of the chosen intervention, combining treatments with targeted rehabilitation ensures the best long-term outcomes. [12] Comprehensive care helps restore movement patterns and reduces the likelihood of symptom recurrence.
Conclusion
Cervical facet joints are a major source of neck pain, especially in individuals with degenerative changes, whiplash injuries, or inflammation of the joint capsule. Because imaging findings alone do not reliably identify facet-mediated pain, clinicians rely on medial branch blocks as the most accurate diagnostic tool. Once a diagnosis is established, patients may benefit from a range of evidence-based interventions including exercise therapy, corticosteroid injections, and radiofrequency ablation. Recognizing the significance of cervical facet joints in neck pain allows for more precise diagnosis and more effective treatment, ultimately improving quality of life for individuals seeking relief.
References
- Cohen SP. Epidemiology, diagnosis, and treatment of neck pain. Mayo Clin Proc. 2015;90(2):284–99.
- Hurley RW, Adams MCB, Barad M, et al. Consensus practice guidelines on interventions for cervical spine (facet) joint pain. Reg Anesth Pain Med. 2022;47(1):3–59.
- Won HS, Kim YD. Cervical facet joint interventions for neck pain: an anatomically and clinically focused review. Anesth Pain Med (Seoul). 2025;20(4):329–40.
- Chen HB, Yang KH, Wang ZG. Biomechanics of whiplash injury. Chin J Traumatol. 2009;12(5):305–14.
- Gellhorn AC, Katz JN, Suri P. Osteoarthritis of the spine: the facet joints. Nat Rev Rheumatol. 2013;9(4):216–24.
- Bogduk N. Neck pain. Aust Fam Physician. 1984;13(1):26–30.
- Farrell S, Smith A, Schneider B, et al. Glucocorticoid facet joint injection for chronic back or neck pain. Cochrane Database Syst Rev. 2024;11:CD015354.
- Suer M, Wahezi SE, Abd-Elsayed A, Sehgal N. Cervical facet joint pain and cervicogenic headache treated with radiofrequency ablation. Pain Physician. 2022;25(3):251–63.
- Gellhorn AC. Cervical facet-mediated pain. Phys Med Rehabil Clin N Am. 2011;22(3):447–58.
- Hu N, Dougherty C. Neck-Tongue Syndrome. Curr Pain Headache Rep. 2016;20(4):27.
- Le DT, Alem N. Facet Joint Injection. StatPearls. 2023–2026.
- Manchikanti L, Hirsch JA, Kaye AD, Boswell MV. Interventional management of cervical facet joint pain. Postgrad Med. 2016;128(1):54–68.
- Cohen SP, Huang JH, Brummett C. Facet joint pain—advances in patient selection and treatment. Nat Rev Rheumatol. 2013;9(2):101–16.
- Yang S, Chang MC. Corticosteroid injection into cervical facet joints for whiplash-related neck pain. Ann Palliat Med. 2022;11(8):2569–73.