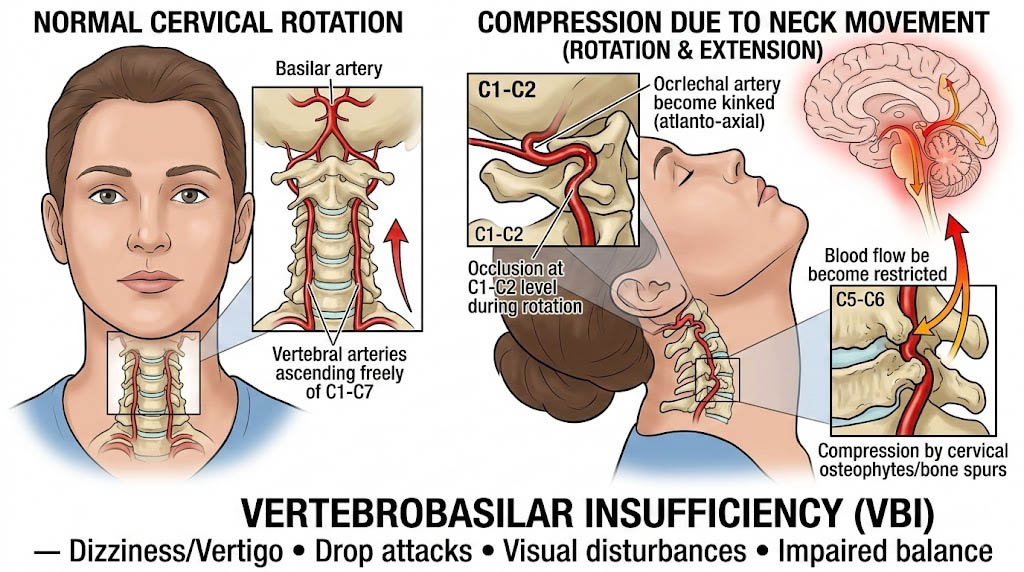
Many medical conditions can cause dizziness and nausea. However, when dizziness occurs during head rotation, particularly when accompanied by diplopia, cervical-related vertebrobasilar insufficiency should be strongly suspected. In such cases, mechanical compromise of the vertebral arteries during cervical movement may reduce blood flow to the posterior circulation of the brain, leading to transient ischemic symptoms.
Overview and Definition
Vertebrobasilar insufficiency (VBI) refers to a clinical condition characterized by inadequate blood flow within the vertebrobasilar arterial system, which supplies the posterior portion of the brain. This vascular territory includes essential structures such as the brainstem, cerebellum, occipital lobes, thalamus, and medial temporal regions. Reduced perfusion in this system can lead to transient ischemic symptoms or permanent neurological damage, depending on the severity and duration of the ischemia. Because these structures are responsible for critical neurological functions including balance, vision, coordination, and autonomic regulation, impaired circulation may produce a broad spectrum of clinical manifestations.[1–3]
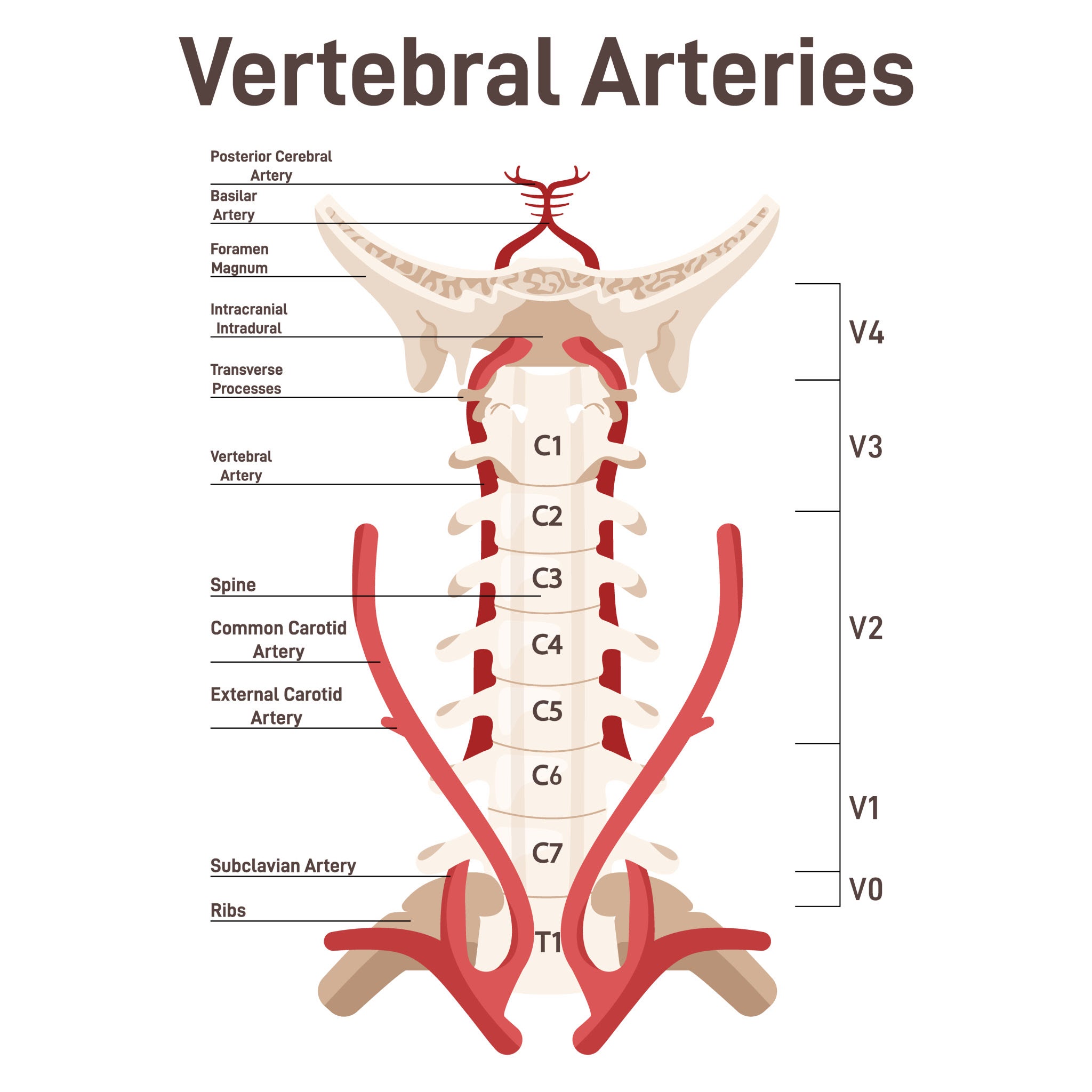
The vertebrobasilar circulation is formed by the two vertebral arteries, which arise from the subclavian arteries and ascend through the transverse foramina of the cervical vertebrae before entering the cranial cavity through the foramen magnum. At the pontomedullary junction, the two vertebral arteries merge to form the basilar artery, which subsequently branches to supply much of the posterior brain. Any pathological condition that interferes with blood flow in these vessels—such as arterial stenosis, thrombosis, embolism, or mechanical compression—may lead to vertebrobasilar insufficiency.[4–6]
Historical Perspectives and Diagnostic Considerations
Historically, the term vertebrobasilar insufficiency has been used rather broadly in clinical practice. In many cases, it has been applied to patients presenting with nonspecific neurological symptoms such as dizziness, imbalance, or blurred vision. However, several investigators have emphasized that the term should be used with caution, as these symptoms may arise from numerous nonvascular conditions. Sturzenegger noted that vertebrobasilar insufficiency is often an imprecise and overused diagnostic label, particularly when it is applied to intermittent symptoms without objective evidence of posterior circulation ischemia. [1]
Similarly, earlier reviews of the literature have suggested that clinical examination alone rarely allows accurate localization of vascular lesions within the posterior circulation. As a result, reliable diagnosis requires a comprehensive evaluation that includes both clinical assessment and imaging studies. [7] Over time, advances in neuroimaging and vascular diagnostics have significantly improved the ability to identify pathological changes within the vertebrobasilar system.
Clinical Manifestations
The clinical manifestations of vertebrobasilar insufficiency are diverse and often reflect dysfunction of the brainstem and cerebellum. Symptoms may occur as transient ischemic attacks or as more persistent neurological deficits. Common manifestations include vertigo, dizziness, diplopia, dysarthria, ataxia, visual disturbances, nausea, vomiting, and in some cases syncope or sudden falls. [4, 8]
Among these symptoms, vertigo is considered one of the most frequent presentations of transient ischemia within the vertebrobasilar circulation. Episodes of vertigo related to vascular insufficiency often begin abruptly and may last from several minutes to hours. These episodes are frequently accompanied by other neurological symptoms, although isolated vertigo may occasionally occur. [4] Repeated transient ischemic episodes can precede more serious neurological events, including cerebellar or brainstem infarction. [8]
Etiology and Risk Factors
The underlying causes of vertebrobasilar insufficiency are varied and involve both vascular and structural abnormalities. One of the most common etiological factors is atherosclerosis affecting the vertebral or basilar arteries. Progressive plaque formation may lead to arterial narrowing and impaired blood flow to the posterior circulation. Vascular risk factors such as hypertension, diabetes mellitus, hyperlipidemia, and smoking contribute significantly to the development of atherosclerotic disease. [8]
Inflammatory processes may also play an important role in the pathogenesis of vertebrobasilar insufficiency. Recent studies have suggested that markers associated with inflammation and oxidative stress, including gamma-glutamyltransferase, may correlate with the presence of vertebrobasilar insufficiency and vascular atherosclerosis. [9] These findings highlight the complex interplay between vascular inflammation and cerebrovascular disease.
Mechanical and Structural Causes
In addition to intrinsic vascular disease, mechanical factors may compromise vertebrobasilar circulation. Degenerative changes of the cervical spine, including osteophyte formation and spondylosis, may compress the vertebral arteries during certain neck movements. In such cases, symptoms of vertebrobasilar insufficiency may occur when the head is rotated or extended, resulting in transient reduction of blood flow. [10]
A well-recognized example of mechanically induced vertebrobasilar insufficiency is rotational vertebral artery syndrome, also known as Bow Hunter’s syndrome. In this condition, head rotation leads to temporary occlusion of the vertebral artery, producing symptoms such as vertigo, visual disturbance, and syncope. [11] Rarely, hypertrophy of cervical muscles or congenital anatomical abnormalities may also contribute to vascular compression and subsequent ischemic symptoms. [11]
Other Vascular Pathologies
Several other vascular conditions may contribute to vertebrobasilar insufficiency. Arterial dissection is an important cause, particularly among younger patients. Dissection involves a tear in the arterial wall that allows blood to enter the vessel wall and form a false lumen, resulting in stenosis or embolic complications. Vertebral or carotid artery dissection may therefore present with symptoms of posterior circulation ischemia. [6]
Additionally, structural abnormalities of the vertebrobasilar arteries, such as dolichoectasia or aneurysmal dilation, may affect cerebral hemodynamics. Dolichoectatic vertebrobasilar arteries are characterized by elongation and dilation of the vessel, which can lead to thromboembolic events or compressive effects on adjacent neural structures. [12] These abnormalities illustrate the diverse spectrum of vascular pathologies that can influence vertebrobasilar circulation.
Diagnostic Approaches
Accurate diagnosis of vertebrobasilar insufficiency requires careful evaluation because the symptoms are often nonspecific and overlap with other neurological or vestibular disorders. Early diagnostic strategies proposed stepwise approaches that incorporated noninvasive screening methods followed by more definitive imaging studies when necessary. [2]
Modern diagnostic techniques rely heavily on imaging modalities that allow visualization of the vertebrobasilar arteries and assessment of cerebral perfusion. Duplex ultrasonography, computed tomography angiography (CTA), and magnetic resonance angiography (MRA) are commonly used to identify arterial stenosis, occlusion, or anatomical abnormalities. In certain cases, digital subtraction angiography remains the gold standard for detailed vascular evaluation. Functional imaging techniques such as single-photon emission computed tomography (SPECT) may also assist in identifying perfusion deficits associated with vertebrobasilar insufficiency. [13]
Management and Treatment Considerations
Management of vertebrobasilar insufficiency depends on the underlying cause and severity of symptoms. Conservative treatment generally focuses on reducing vascular risk factors and preventing thromboembolic complications. Medical therapy often includes antiplatelet agents, blood pressure control, lipid-lowering medications, and lifestyle modifications aimed at improving cardiovascular health. [8]
For patients with severe vascular stenosis or persistent ischemic symptoms despite medical therapy, surgical or endovascular interventions may be considered. Various procedures have been developed to restore adequate blood flow in the vertebrobasilar circulation, including bypass surgery, endarterectomy, and other revascularization techniques. [14] Recent advances in vascular surgery and endovascular technology have expanded treatment options for patients with complex vertebrobasilar disease. [15]
Summary
Vertebrobasilar insufficiency represents a complex cerebrovascular condition resulting from reduced blood flow within the posterior circulation of the brain. It may arise from a wide range of etiologies, including atherosclerotic vascular disease, arterial dissection, mechanical compression, and congenital vascular abnormalities. The clinical presentation is often variable, ranging from transient dizziness and visual disturbances to severe neurological deficits and stroke. Because of the nonspecific nature of many symptoms, accurate diagnosis requires careful clinical assessment supported by modern imaging techniques. Early recognition and appropriate management are essential to prevent recurrent ischemic episodes and reduce the risk of posterior circulation stroke.
References
- Sturzenegger M. Vertebrobasilar insufficiency. Schweiz Med Wochenschr. 1997;127(40):1658-62.
- Valvassori G, Dobben GD. Vertebrobasilar insufficiency. Ann Otol Rhinol Laryngol. 1979;88(5 Pt 1):689-92.
- McGuire LS, Charbel FT. A narrative review of techniques for surgical revascularization of the extracranial vertebral artery in vertebrobasilar insufficiency. Neurochirurgie. 2024;70(3):101516.
- Baloh RW. Vertebrobasilar insufficiency and stroke. Otolaryngol Head Neck Surg. 1995;112(1):114-7.
- Rieben FW. Vertebrobasilar insufficiency. Dtsch Med Wochenschr. 1980;105(38):1302-3.
- Costello F. Carotid artery dissection and vertebrobasilar insufficiency. Int Ophthalmol Clin. 2009;49(3):1-14.
- Ausman JI, Shrontz CE, Pearce JE, Diaz FG, Crecelius JL. Vertebrobasilar insufficiency: a review. Arch Neurol. 1985;42(8):803-8.
- Savitz SI, Caplan LR. Vertebrobasilar disease. N Engl J Med. 2005;352(25):2618-26.
- Ulu MS, Beker-Acay M, Ulu S, Unlu E, Bucak A, Yaman G, et al. Vertebrobasilar insufficiency and gamma-glutamyltransferase: an emerging relationship demonstrating inflammation and atherosclerosis. Bratisl Lek Listy. 2016;117(8):448-52.
- Yang YJ, Chien YY, Cheng WC. Vertebrobasilar insufficiency related to cervical spondylosis: a case report and review of the literature. Changgeng Yi Xue Za Zhi. 1992;15(2):100-4.
- Sarkar J, Wolfe SQ, Ching BH, Kellicut DC. Bow hunter's syndrome causing vertebrobasilar insufficiency in a young man with neck muscle hypertrophy. Ann Vasc Surg. 2014;28(4):1032.e1-1032.e10.
- Rezai Jahromi B, Niemelä M. Dolichoectatic vertebrobasilar artery aneurysms. Neurosurg Clin N Am. 2022;33(4):419-429.
- Cagnie B, Vinck E, Cambier D. The role of SPECT imaging in the diagnosis of vertebrobasilar insufficiency. Nucl Med Commun. 2005;26(4):299-301.
- Britz GW, Agarwal V, Mihlon F, Ramanathan D, Agrawal A, Nimjee SM, et al. Radial artery bypass for intractable vertebrobasilar insufficiency: case series and review of the literature. World Neurosurg. 2016;85:106-13.
- Shurkhay V, King BL, Acuff NJ, Neel J, Kalani MYS. Transcervical vertebral artery origin endarterectomy for vertebrobasilar insufficiency. World Neurosurg. 2024;184:14.