Idiopathic scoliosis is the most common form of spinal curvature disorder affecting children and adolescents. The condition is characterized by a three-dimensional deformity of the spine in which the vertebral column deviates laterally and rotates along its axis. Clinically, scoliosis is defined as a lateral curvature of the spine measuring 10 degrees or more on the Cobb angle on radiographic examination in the absence of identifiable congenital, neuromuscular, or syndromic causes[1,8]. Although scoliosis can occur at any age, the majority of cases are diagnosed during adolescence, when rapid skeletal growth occurs.
Idiopathic scoliosis accounts for the vast majority of scoliosis cases in the pediatric population. Among adolescents, it represents approximately 80–90% of all scoliosis diagnoses[6,15]. The prevalence of adolescent idiopathic scoliosis (AIS) is estimated to range between 1% and 3% of adolescents, although many mild cases remain undiagnosed because symptoms may be minimal in the early stages[1]. The condition affects both sexes; however, girls are more likely than boys to develop progressive spinal curves requiring clinical management.
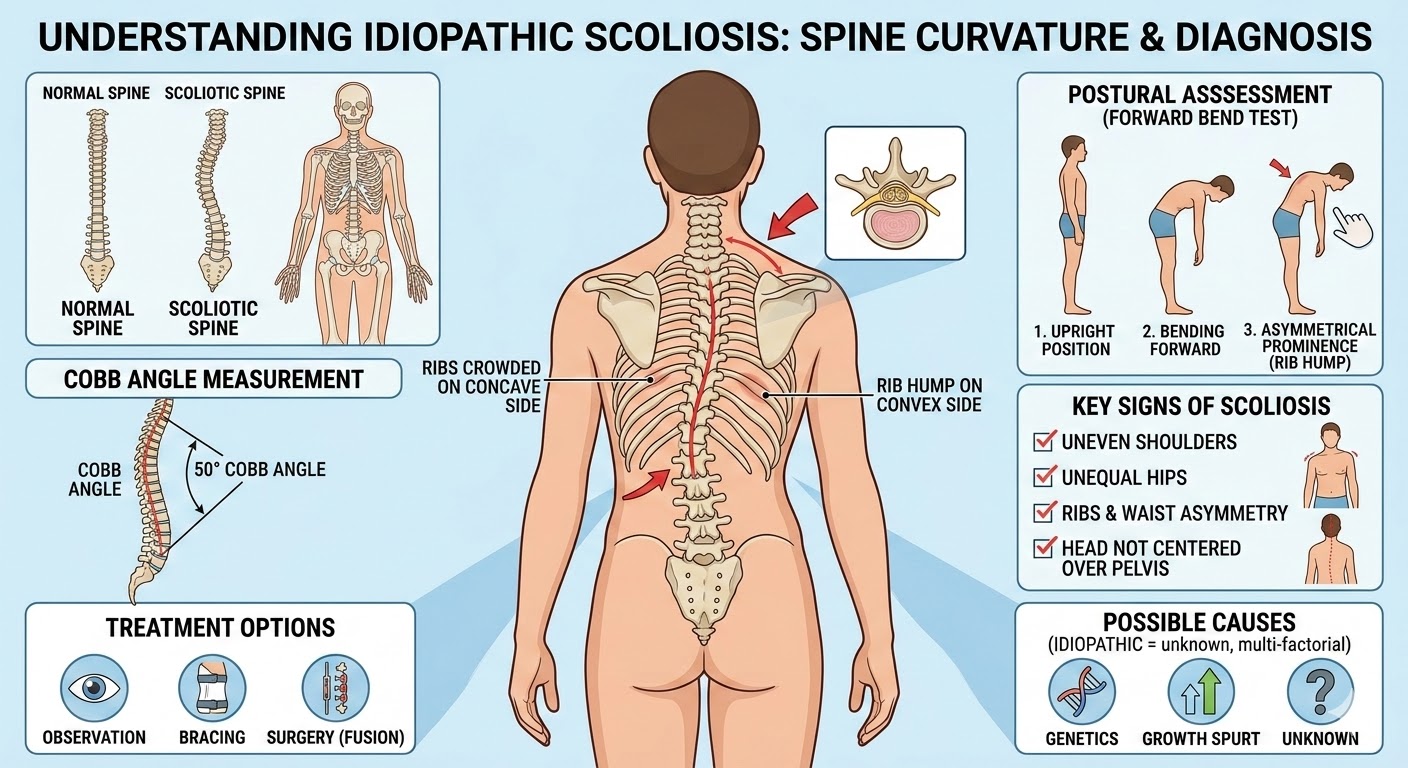
Understanding the Nature of Idiopathic Scoliosis
Idiopathic scoliosis is considered a three-dimensional structural deformity rather than a simple sideways curvature of the spine. In addition to lateral deviation, the vertebrae often rotate, which may produce visible asymmetry of the trunk. This rotation can lead to uneven shoulders, rib prominence, asymmetry of the waist, or imbalance of the pelvis when the condition progresses[3].
Unlike congenital scoliosis, which results from vertebral malformations present at birth, or neuromuscular scoliosis associated with conditions such as cerebral palsy or muscular dystrophy, idiopathic scoliosis is diagnosed primarily by excluding identifiable causes[2]. Because the underlying mechanism remains unclear, the term “idiopathic” is used to describe the condition.
The development of idiopathic scoliosis can occur during different growth stages, leading to classification into infantile, juvenile, and adolescent forms. Infantile idiopathic scoliosis appears before the age of three years, juvenile scoliosis occurs between ages three and ten, and adolescent idiopathic scoliosis is diagnosed between the ages of eleven and eighteen[12]. Among these types, AIS is by far the most common presentation encountered in clinical practice.
Epidemiology and Risk Factors
Adolescent idiopathic scoliosis most frequently develops during periods of rapid skeletal growth. The progression of spinal curvature often corresponds with the adolescent growth spurt, suggesting that growth-related factors play an important role in the development and progression of the condition[6].
Several risk factors have been associated with curve progression. These include younger age at diagnosis, female sex, skeletal immaturity, and larger initial Cobb angles[1]. The natural history of idiopathic scoliosis varies considerably. Many mild curves remain stable throughout growth and require only observation, while more significant curves may gradually worsen and require active intervention.
Genetic influences are believed to contribute significantly to the development of idiopathic scoliosis. Family studies and genetic research have demonstrated increased incidence among relatives of affected individuals, suggesting a hereditary component[5]. However, no single gene has been identified as the sole cause, and the disorder is generally considered multifactorial, involving interactions between genetic, biomechanical, neurological, and hormonal factors.
Current Theories of Etiology
Despite decades of research, the exact cause of idiopathic scoliosis remains unknown. Several theories have been proposed to explain the pathogenesis of the condition, and current evidence suggests that multiple mechanisms may interact in susceptible individuals.
One important area of investigation involves abnormal spinal growth and biomechanical imbalance. Rapid vertebral growth during adolescence may create asymmetrical loading patterns within the spine, leading to progressive curvature and rotation[5].
Neurological factors have also been explored. Some studies suggest that dysfunction within the vestibular system, which contributes to balance and spatial orientation, may play a role in spinal asymmetry and postural control in individuals with scoliosis[16]. Altered sensory integration and neuromuscular control may influence spinal alignment during growth.
Hormonal influences have also been proposed as contributing factors. Research examining the role of melatonin, a hormone involved in circadian rhythm regulation, suggests that abnormalities in melatonin signaling may affect spinal growth and musculoskeletal development in some individuals with AIS[13].
Additionally, environmental and lifestyle factors have been investigated. Physical activity patterns may influence spinal development, although current evidence does not establish a clear causal relationship between activity levels and scoliosis onset[7]. Overall, idiopathic scoliosis is best understood as a complex multifactorial disorder involving interactions between biological, mechanical, and environmental influences.
Clinical Presentation and Diagnosis
In many cases, idiopathic scoliosis develops gradually and may not cause pain or noticeable symptoms in its early stages. Instead, the condition is often first recognized through postural changes, such as uneven shoulders, asymmetry of the rib cage, or differences in waist contour. A prominent rib hump during forward bending is a common clinical sign caused by vertebral rotation.
Screening examinations, including the Adams forward bend test, are frequently used in school or clinical settings to identify potential spinal asymmetry. If scoliosis is suspected, radiographic imaging is performed to measure the Cobb angle and confirm the diagnosis[1].
Radiographic assessment not only confirms the presence of scoliosis but also helps determine the severity and progression risk of the spinal curvature. Curves are typically categorized as mild, moderate, or severe based on Cobb angle measurements. Monitoring progression is particularly important during adolescence, when rapid growth may lead to worsening of the deformity.
Management Approaches
The management of idiopathic scoliosis depends primarily on the severity of the curve and the risk of progression. Many mild cases require only regular monitoring during growth. Observation with periodic clinical and radiographic evaluation is often recommended when curves are small and stable[14].
For moderate curves in growing adolescents, non-surgical treatment may be recommended to prevent further progression. Bracing is commonly used in this stage to help stabilize the spine and reduce the risk of curve progression during growth[15].
Exercise-based interventions have also received increasing attention in scoliosis management. Specific physiotherapy programs, including scoliosis-specific exercises and core stabilization training, aim to improve spinal alignment, muscular balance, and postural control. Research suggests that targeted exercise programs may contribute to improved functional outcomes and spinal stability when incorporated into conservative treatment plans[9,10].
In severe cases where spinal curvature continues to progress despite conservative treatment, surgical intervention may be considered to correct deformity and restore spinal balance. Modern surgical techniques aim to achieve effective correction while preserving spinal mobility and minimizing complications[15].
Living with Idiopathic Scoliosis
Although idiopathic scoliosis can affect spinal alignment and body symmetry, many individuals with mild to moderate curves live active and healthy lives. Early detection, appropriate monitoring, and individualized management strategies play an important role in maintaining spinal health and preventing progression.
Healthcare providers increasingly emphasize a multidisciplinary approach, incorporating medical evaluation, physiotherapy, and supportive care to optimize long-term outcomes. Education about posture, physical activity, and spinal awareness can also help individuals better manage their condition.
As research continues, a deeper understanding of the biological mechanisms underlying idiopathic scoliosis may lead to improved prevention strategies and more personalized treatment options in the future.
References
- Kuznia AL, Hernandez AK, Lee LU. Adolescent idiopathic scoliosis: Common questions and answers. Am Fam Physician. 2020;101(1):19-23.
- Yaman O, Dalbayrak S. Idiopathic scoliosis. Turk Neurosurg. 2014;24(5):646-657.
- Addai D, Zarkos J, Bowey AJ. Current concepts in the diagnosis and management of adolescent idiopathic scoliosis. Childs Nerv Syst. 2020;36(6):1111-1119.
- Almahmoud OH, Baniodeh B, Musleh R, et al. Overview of adolescent idiopathic scoliosis and associated factors: A scoping review. Int J Adolesc Med Health. 2023;35(6):437-441.
- Peng Y, Wang SR, Qiu GX, Zhang JG, Zhuang QY. Research progress on the etiology and pathogenesis of adolescent idiopathic scoliosis. Chin Med J. 2020;133(4):483-493.
- Marya S, Tambe AD, Millner PA, Tsirikos AI. Adolescent idiopathic scoliosis: A review of aetiological theories of a multifactorial disease. Bone Joint J. 2022;104-B(8):915-921.
- Qi X, Peng C, Fu P, Zhu A, Jiao W. Correlation between physical activity and adolescent idiopathic scoliosis: A systematic review. BMC Musculoskelet Disord. 2023;24(1):978.
- Angevine PD, Deutsch H. Idiopathic scoliosis. Neurosurgery. 2008;63(3 Suppl):86-93.
- Yagci G, Yakut Y. Core stabilization exercises versus scoliosis-specific exercises in moderate idiopathic scoliosis treatment. Prosthet Orthot Int. 2019;43(3):301-308.
- Gür G, Ayhan C, Yakut Y. The effectiveness of core stabilization exercise in adolescent idiopathic scoliosis: A randomized controlled trial. Prosthet Orthot Int. 2017;41(3):303-310.
- Zhang X, Dai X, Chen Y, Yang H. Adolescent idiopathic scoliosis: A case report and review of experiences. Asian J Surg. 2024;47(10):4548-4549.
- Lincoln TL. Infantile idiopathic scoliosis. Am J Orthop. 2007;36(11):586-590.
- Gargano G, Oliva F, Migliorini F, Maffulli N. Melatonin and adolescent idiopathic scoliosis: The present evidence. Surgeon. 2022;20(6):e315-e321.
- Roach JW. Adolescent idiopathic scoliosis. Orthop Clin North Am. 1999;30(3):353-365.
- Cheung ZB, Selverian S, Cho BH, Ball CJ, Cho SK. Idiopathic scoliosis in children and adolescents: Emerging techniques in surgical treatment. World Neurosurg. 2019;130:e737-e742.
- Hawasli AH, Hullar TE, Dorward IG. Idiopathic scoliosis and the vestibular system. Eur Spine J. 2015;24(2):227-233.