Spasmodic torticollis, also known as cervical dystonia, is a chronic neurological condition characterized by involuntary, recurrent, or sustained contractions of the cervical musculature leading to abnormal head posture, pain, and functional disability. The disorder has been recognized throughout medical history, yet its pathophysiology and optimal clinical management continue to evolve. Early reports from major medical journals described it primarily as a disabling and psychologically distressing condition affecting adults in mid-life, frequently resulting in significant social and occupational impairment. Subsequent work refined the definition and recognized the central role of basal ganglia dysfunction and abnormal sensorimotor integration in disease expression.
Prevalence
Spasmodic torticollis is the most common form of focal dystonia. Epidemiological data estimate its prevalence to be approximately 30 to 60 cases per million people, though rates vary between regions and depend on diagnostic criteria. Earlier clinical observations noted that women are affected more frequently than men, with onset most often occurring between the ages of 30 and 60 years3. Because mild or atypical presentations may go unrecognized, true prevalence is likely higher. Advances in diagnostic methods as well as greater public and clinical awareness have contributed to increased detection compared to earlier decades when the disorder was often misclassified as psychogenic9.
Etiology
The etiology of spasmodic torticollis is multifactorial. Historically, some early publications reported psychological factors, emotional distress, or personality features as contributing elements, reflecting the prevailing psychogenic interpretation of dystonia during that era6. However, modern research strongly supports a neurological origin. Abnormalities in basal ganglia circuits, sensorimotor integration, and cortical inhibition have been demonstrated in neurophysiological and imaging studies, indicating that dystonia arises from dysfunctional motor control rather than primary psychiatric causes7.
Idiopathic cervical dystonia remains the most common form, where no structural lesion or genetic mutation is identifiable. Secondary forms may arise from trauma, peripheral nerve injury, neuroleptic exposure, or structural brain abnormalities, though these account for a minority of cases. Surgical literature has also examined cervical nerve anomalies and hyperactive motor branches, suggesting that peripheral motor input may exacerbate centrally mediated dystonia in some individuals5. Overall, the etiology is best understood as an interplay between genetic predisposition, central motor network dysfunction, and peripheral feedback mechanisms.
Clinical Features: Signs and Symptoms
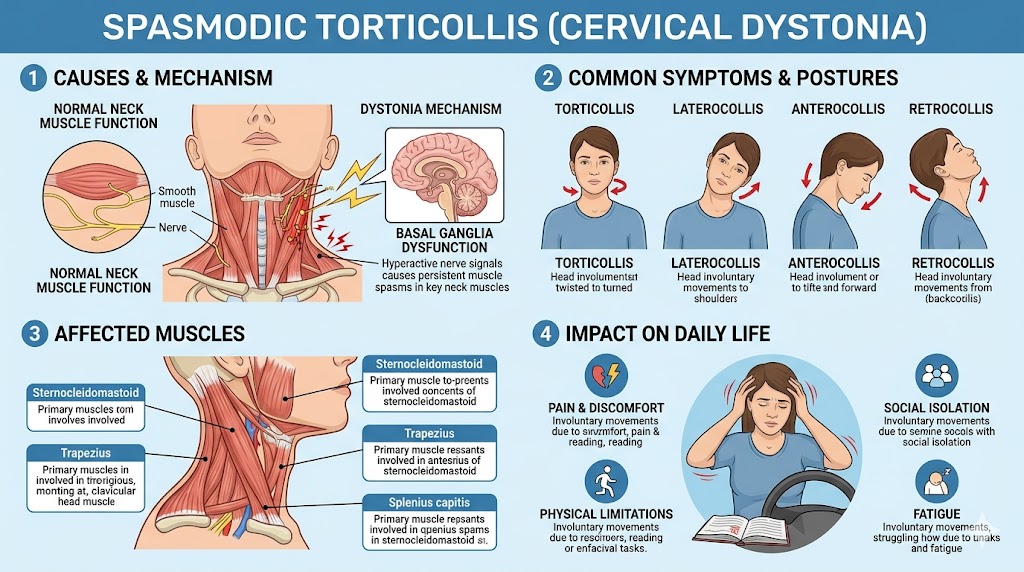
Patients with spasmodic torticollis typically present with involuntary neck muscle contractions producing abnormal head positions such as rotation (torticollis), lateral tilt (laterocollis), flexion (anterocollis), or extension (retrocollis). Some individuals display mixed patterns. Pain is a prominent symptom and often the most disabling aspect of the condition. Early reports documented that pain may radiate from the cervical spine into the shoulders and upper back and may fluctuate with emotional stress or fatigue1.
Another characteristic feature is the presence of sensory tricks, or “geste antagoniste,” where gentle touch to certain areas such as the chin or the side of the face temporarily reduces the involuntary movements. Although these maneuvers do not correct underlying dysfunction, they provide important diagnostic clues. Patients may also report tremor, jerky movements, hypertrophy of overactive muscles, and functional limitations in activities requiring stable head positioning. Over time, chronic abnormal postures can lead to secondary musculoskeletal changes including facet joint irritation, muscle imbalance, and degenerative cervical spine changes.
Diagnosis
Diagnosis is primarily clinical and based on recognition of characteristic involuntary contractions and abnormal head postures. A detailed neurological and musculoskeletal examination is essential to distinguish dystonia from other causes of torticollis such as congenital muscular imbalance, acute cervical muscle spasm, infections, fractures, or atlantoaxial pathology. Early literature emphasized the need to differentiate spasmodic torticollis from psychiatric disorders, given that misdiagnosis was historically common9. Modern guidelines integrate neurological examination with optional adjunct testing such as electromyography to identify the pattern of muscle overactivity.
Imaging is not routinely required but may be indicated when symptoms are atypical or when trauma or structural abnormalities are suspected. Response to sensory tricks and the chronic, patterned nature of symptoms supports the diagnosis of cervical dystonia. Because the condition can mimic musculoskeletal dysfunction, clinicians must carefully assess active and passive cervical ranges of motion, palpate for focal muscle activity, and evaluate for compensatory thoracic or shoulder girdle patterns. Osteopathic structural examination can further identify secondary somatic dysfunctions that contribute to symptom persistence.
Management
Management of spasmodic torticollis is multidisciplinary and involves pharmacologic, rehabilitative, procedural, surgical, and osteopathic approaches. Historically, treatment options were limited, and many patients experienced persistent disability. Early clinical accounts described the use of sedatives, anticholinergics, and psychotherapy, though these methods demonstrated inconsistent efficacy4. Modern management strategies are more effective and grounded in neurophysiological understanding.
Botulinum toxin injection is now the first-line treatment for most patients. It works by reducing excessive muscle contractions through temporary chemodenervation of overactive cervical muscles. Multiple clinical series and long-term follow-up studies have demonstrated its safety and effectiveness, with significant improvement in pain and function for the majority of patients10. Injection planning typically incorporates EMG guidance or ultrasound to identify the most active muscles.
Oral medications such as anticholinergics, benzodiazepines, or muscle relaxants may be used as adjuncts but generally offer limited benefit. Physical therapy focuses on stretching shortened muscles, improving postural alignment, and retraining motor patterns. Because the condition involves abnormal sensorimotor integration, therapies emphasizing proprioception and controlled movement may provide meaningful symptom relief.
Osteopathic Management
Osteopathic treatment can play a complementary role by reducing secondary musculoskeletal strain, improving biomechanical balance, and addressing somatic dysfunctions resulting from chronic abnormal posture. Soft tissue techniques may help decrease hypertonicity in overactive muscles such as the sternocleidomastoid, splenius capitis, levator scapulae, and upper trapezius. Myofascial release can improve cervical and upper thoracic mobility, while counterstrain and muscle energy techniques may help normalize dysfunctional muscle spindles and improve controlled range of motion. Although osteopathic manipulative treatment does not address the primary neurological etiology, it can substantially reduce pain, improve functional mobility, and augment the effects of botulinum toxin by optimizing biomechanics and reducing compensatory patterns.
High-velocity low-amplitude (HVLA) manipulation is typically avoided or used cautiously, particularly in patients with significant muscle spasm or degenerative cervical spine changes. Gentle indirect methods are generally preferred. Integration of breathing techniques and postural retraining may further enhance outcomes. Osteopathic physicians often coordinate care with neurologists to optimize timing relative to botulinum toxin cycles, ensuring manipulative therapy supports movement retraining when muscle overactivity is reduced.
Surgical Management
Surgical intervention is reserved for refractory cases. Historical procedures included peripheral nerve sectioning and rhizotomy, which provided inconsistent results and risked significant complications12. Contemporary surgical approaches have improved significantly. Modern nerve dissection techniques aim to selectively interrupt hyperactive motor branches while preserving function, offering better outcomes and fewer adverse effects5. In severe cases, deep brain stimulation of the globus pallidus internus has been explored, although this is more common in generalized dystonia than in isolated torticollis.
Prognosis
The prognosis of spasmodic torticollis varies, though most patients experience chronic symptoms with fluctuating severity. Early reports noted that spontaneous remission occurs in a minority of individuals, often within the first several years of symptom onset3. With modern treatment, particularly botulinum toxin injection combined with rehabilitative and osteopathic strategies, many patients achieve meaningful symptom control. Pain and disability typically diminish, though complete cure is uncommon.
Prevention
There is no known method to prevent idiopathic spasmodic torticollis, as the underlying neurological dysfunction is not fully understood. Preventive strategies center on early recognition, prompt treatment, and reduction of secondary musculoskeletal complications. Patients benefit from maintaining ergonomic posture, minimizing repetitive strain, and engaging in regular cervical and thoracic mobility exercises. Osteopathic care can help prevent chronic compensatory dysfunction, while ongoing neurologic follow-up ensures timely adjustment of therapeutic strategies.
References
1. No authors listed. Spasmodic torticollis. Br Med J. 1978 Sep 16;2(6140):786.
2. Duane DD. Spasmodic torticollis. Adv Neurol. 1988;49:135-150.
4. No authors listed. Spasmodic torticollis. Lancet. 1978 Aug 5;2(8084):301-302.
10. Moore AP. Spasmodic torticollis. BMJ. 1988 Jul 16;297(6642):201. doi: 10.1136/bmj.297.6642.201.