Scoliosis is a three-dimensional spinal deformity involving lateral curvature and vertebral rotation. Although it can occur at any age, the most common form—adolescent idiopathic scoliosis (AIS)—typically appears between ages 10 and 16. Studies estimate a prevalence of 2% to 4% of adolescents, with many cases being mild and asymptomatic [1, 4]. Early identification improves monitoring and helps determine whether a child requires observation, bracing, or further evaluation.
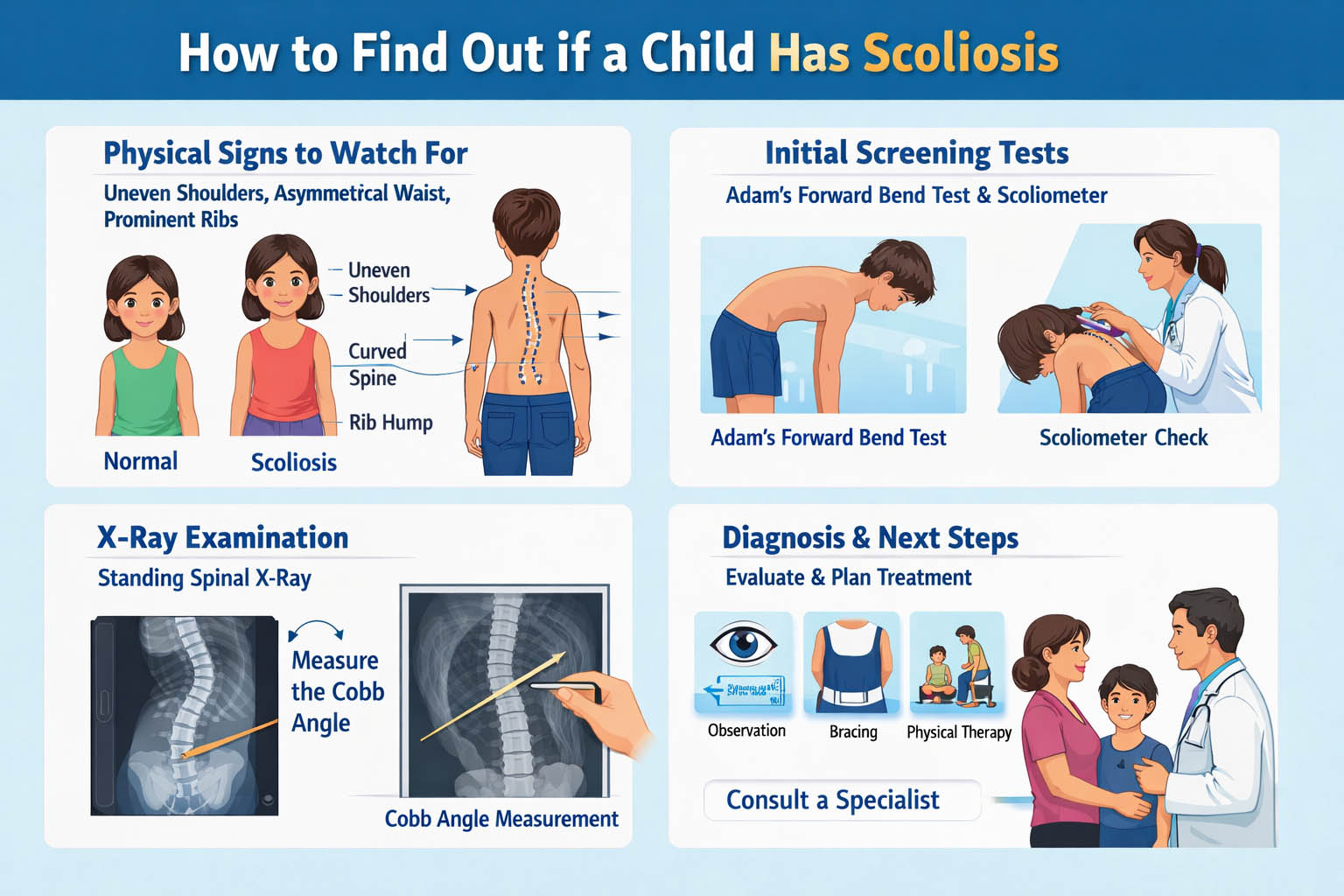
This webpage explains how parents and clinicians can identify scoliosis through physical signs, screening tests, and imaging. It also illustrates the Cobb angle, the most widely used radiographic measurement to assess curve severity.
Common Signs That Suggest Scoliosis
- Uneven shoulders (one appears higher)
- Prominent shoulder blade
- Uneven waistline
- One hip appearing higher or more pronounced
- Clothes hanging unevenly
- Leaning to one side when standing
These physical signs alone cannot confirm scoliosis but indicate the need for proper screening.
Initial Screening: The Forward Bend Test
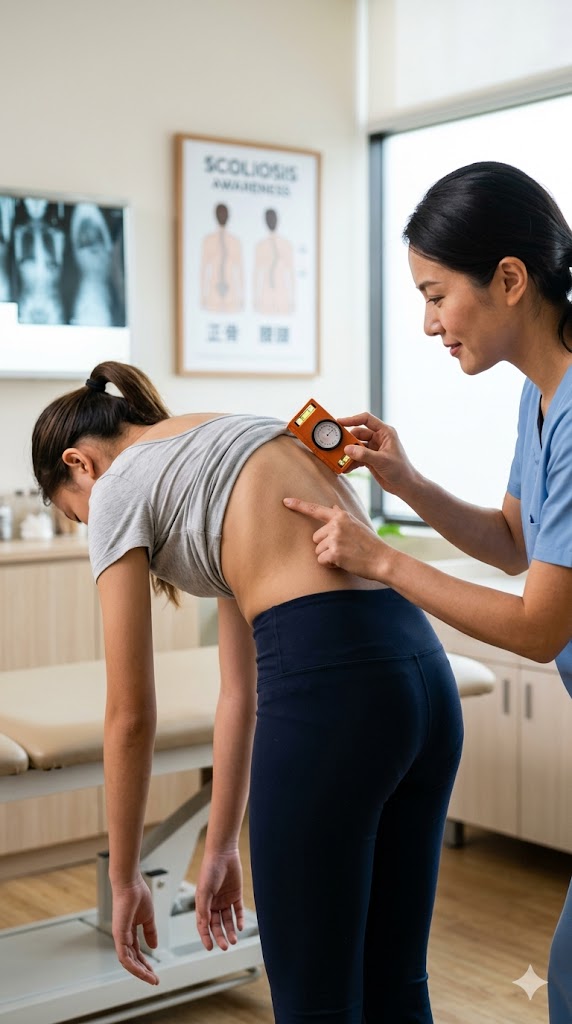
The **Adam’s Forward Bend Test** is a widely used clinical maneuver for scoliosis detection [8]. The child stands with feet together and bends forward at the waist with arms hanging freely. The examiner looks for rib prominence or muscular asymmetry caused by vertebral rotation.
When to Seek X-ray Imaging
- Visible trunk asymmetry with positive forward bend test
- Scoliometer reading ≥ 5–7 degrees
- Rapid growth phase (typically ages 10–14)
- Family history of scoliosis
- Red flags such as neurological symptoms or severe pain
The X-ray enables measurement of the Cobb angle, which defines scoliosis (≥ 10 degrees) and determines severity and treatment options.
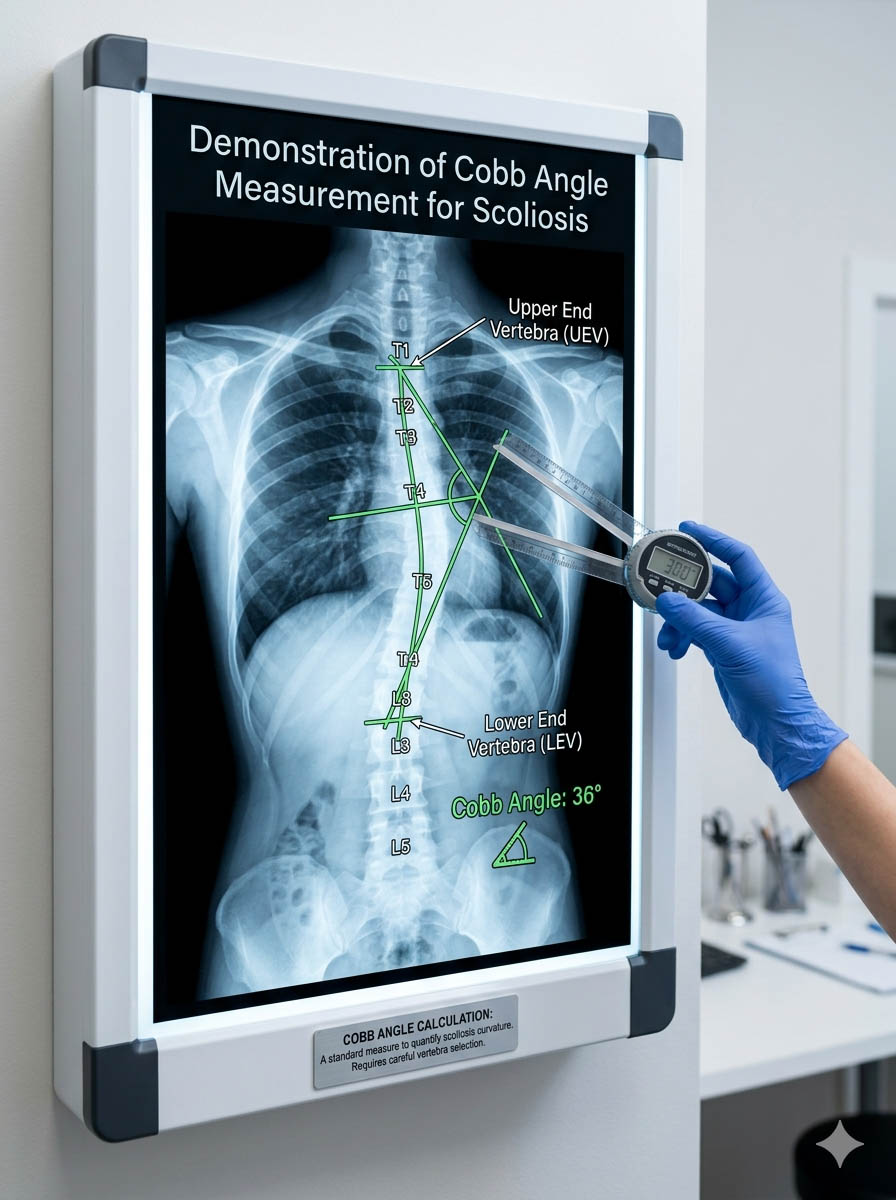
Understanding the Cobb Angle Measurement
- Identify the uppermost and lowest vertebrae that tilt maximally toward the curve apex.
- Draw a line along the superior endplate of the upper vertebra.
- Draw a line along the inferior endplate of the lower vertebra.
- Construct perpendicular lines from both.
- The intersection angle is the Cobb angle.
A Cobb angle of:
- 10–19 degrees: mild scoliosis, usually monitored
- 20–39 degrees: moderate scoliosis, may require bracing
- ≥ 40 degrees: severe scoliosis, may require specialist referral
Red Flags Requiring Specialist Referral
- Onset before age 10
- Neurological deficits
- Severe or localized spinal pain
- Left thoracic curves (atypical pattern)
- Rapid progression despite treatment
When red flags exist, MRI is recommended to evaluate for congenital, neurological, or structural disorders.
Conclusion
Scoliosis in children is common, often subtle, and usually asymptomatic. Parents and clinicians can identify early signs through visual observation, the forward bend test, and scoliometer screening. Radiographic confirmation with Cobb angle measurement remains the diagnostic standard. Understanding these steps helps ensure timely monitoring and appropriate care, minimizing long-term progression and functional impact.
References
- Horne JP, Flannery R, Usman S. Adolescent idiopathic scoliosis: diagnosis and management. Am Fam Physician. 2014;89(3):193-8.
- Kuznia AL, Hernandez AK, Lee LU. Adolescent Idiopathic Scoliosis: Common Questions and Answers. Am Fam Physician. 2020;101(1):19-23.
- Trobisch P, Suess O, Schwab F. Idiopathic scoliosis. Dtsch Arztebl Int. 2010;107(49):875-83.
- Reamy BV, Slakey JB. Adolescent idiopathic scoliosis: review and current concepts. Am Fam Physician. 2001;64(1):111-6.
- Lacroix M, Khalifé M, Ferrero E, Clément O, Nguyen C, Feydy A. Scoliosis. Semin Musculoskelet Radiol. 2023;27(5):529–44.
- Burton MS. Diagnosis and treatment of adolescent idiopathic scoliosis. Pediatr Ann. 2013;42(11):224-8.
- Roach JW. Adolescent idiopathic scoliosis. Orthop Clin North Am. 1999;30(3):353-65.
- Lonstein JE. Adolescent idiopathic scoliosis: screening and diagnosis. Instr Course Lect. 1989;38:105-13.
- Büyükturan Ö, Kaya MH, Alkan H, Büyükturan B, Erbahçeci F. Comparison of Schroth and Lyon exercise techniques in AIS. Musculoskelet Sci Pract. 2024;72:102952.
- Bleck EE. Adolescent idiopathic scoliosis. Dev Med Child Neurol. 1991;33(2):167–73.
- Van Goethem J, Van Campenhout A, van den Hauwe L, Parizel PM. Scoliosis. Neuroimaging Clin N Am. 2007;17(1):105–15.